Fasting can mean anything from total abstinence from food and beverages to restricting specific foods or the hours of food intake. Many religions have traditions of fasting, with various restrictions. There is a good summary of those traditions on Wikipedia. The reason for religious fasting is not to improve health, but for other reasons like improving discipline and demonstrating devotion.
There are many health claims for different fasting regimens. Daily calorie restriction has been demonstrated to prolong lifespans in several organisms, from yeast and worms to mice and monkeys, although the evidence for monkeys is equivocal and there is no evidence for humans. There is some evidence that intermittent fasting can forestall and even reverse cancer, cardiovascular disease, diabetes, and neurodegenerative disorders in mice. In humans, there is some evidence that it might help reduce obesity, hypertension, asthma, and rheumatoid arthritis. How good is the evidence?
Two good reviews of the evidence for fasting
There is a good summary of the relevant research on intermittent fasting here. That article also covers the physiologic and metabolic responses to fasting and argues that they ought to lead to improvement in health. I won’t go into the details here. You can read the article if you want to know more. It’s complicated. Basically, intermittent fasting has potential benefits for anti-aging, cancer, cognitive function, inflammation, hypertension, and the metabolic syndrome; but the evidence so far is insufficient to justify making clinical recommendations.
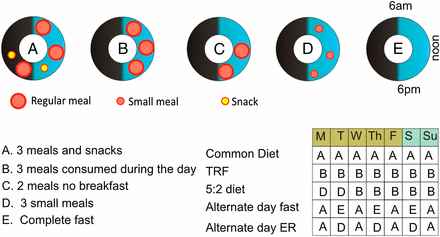
Another recent review article examines the physiologic reactions to the following regimens in animals and humans:
- Calorie restriction (CR) of 20-40% with 3 meals a day
- Intermittent energy restriction (IER), e.g., reduce to 500 calories a day on 2 days a week
- Alternate day fasting (ADF – food only every other day)
- Time-restricted feeding (TRF) (intake limited to a 4-6 hour window)
They point out evolutionary arguments that support fasting: eating patterns of mammals typically involve intermittent energy intake, not three meals a day. Evolution did not prepare us for the modern lifestyle of widely availability high calorie foods and sedentary habits; this lifestyle makes us susceptible to obesity and various diseases. We might do better to eat intermittently like our ancestors did.
They also cover circadian rhythms, which are disrupted by artificial lighting and shift work. There is evidence that this contributes to ill health. There is a circadian rhythm to hunger, with a trough in the morning and a peak in the evening. So maybe eating breakfast isn’t “natural” and isn’t as essential as we have been led to believe.
So far, human studies of fasting in overweight and normal weight subjects have produced mixed results, with generally more favorable results for the obese. Genetic factors may predict which individuals will benefit. The authors conclude:
Further studies are required… As findings from basic research studies and controlled interventional trials accrue, consensus recommendations for healthy patterns of meal frequency and diurnal timing may eventually emerge. If sufficient evidence does emerge to support public health and clinical recommendations to alter meal patterning, there will be numerous forces at play in the acceptance or resistance to such recommendations.
Other considerations regarding fasting
Various fasting regimens have been recommended to aid weight loss, and it seems logical that not eating during some periods would tend to decrease total calorie intake. But a 2003 mouse study found that every-other-day fasting had benefits that were not related to total calorie intake. The mice’s overall food intake did not decrease, and their body weight did not change, but their glucose and insulin levels were reduced and their neurons became more resistant to excitotoxic stress.
A 2014 study in mice found that prolonged fasting (48 hours) promoted stem-cell-based regeneration of the hematopoietic system after damage from chemotherapy by downregulating IGF-1 and PKA activity. The authors speculated that their findings might have significance for human aging and disease. More studies will be needed before it can be recommended to humans. They cautioned that fasting might not be safe for patients who were underweight or had risk factors like diabetes. And fasting can result in headaches and drops in blood pressure that might make driving dangerous.
A 2007 review of studies of alternate day fasting (ADF) found discrepancies between human and animal studies, and could only conclude that:
ADF may effectively modulate metabolic and functional risk factors, thereby preventing or delaying the future occurrence of common chronic diseases, at least in animal models. The effect of ADF on chronic disease risk in normal-weight human subjects remains unclear, however, as do the mechanisms of action. Much work remains to be done to understand this dietary strategy fully.
Joe Mercola recommends fasting, which is worrisome. His website is on the “top 10 worst anti-science websites” list.
Concerns about fasting
Concerns have been raised about various possible adverse effects. It might lower glucose tolerance in women. It might increase blood pressure and cholesterol levels. Some people have gained weight on ADF. It might contribute to eating disorders and create an unhealthy obsession with food. It increases stress and elevates cortisol levels. People on the diet are not fun to be around. Since coffee is allowed, it could lead to overindulgence in caffeine, insomnia, etc. It might increase food intolerances and inflammation. These are largely just speculations not yet supported by any evidence.
Conclusions: Fasting might help, maybe
- People who can tolerate periods of hunger might find intermittent fasting helpful for weight loss; it is simpler to not eat than to try to decide what to eat.
- Although some of the evidence for intermittent fasting sounds promising, we don’t yet know whether it will prolong life or improve health.
- It may be OK to skip breakfast.
- We don’t yet know what the optimum meal frequency and timing are in health or in disease.
- More research is needed, particularly well-designed human trials comparing various fasting regimens to the traditional three meals a day.