A correspondent e-mailed me, saying:
I received my latest issue of Consumer Reports with great interest because the cover story is about back pain. However after reading the article I walked away disappointed. How this well respected publication printed such a poorly researched and written story is unbelievable.
He sent me three related articles that he found objectionable. I did too. They sounded more like popularity contests than science.
The first article: Nondrug treatments should be tried first
The first article starts with an anecdote about a patient who uses acupuncture, tai chi, yoga, massage, and chiropractic for his back pain, mostly paid for by the VA. One can only wonder why he has to use so many different treatments, how effective each is, and whether some of them might be eliminated. One might also wonder why the VA is spending our taxpayer money on treatments of questionable efficacy.
It goes on to cite the guidelines published by the American College of Physicians, saying the first line of defense should be nondrug measures. I heartily agree: that’s just common sense. They say it is backed up by a Consumer Reports survey of 3,542 back-pain sufferers; that survey found that more than 80 percent of those who said they had tried yoga or tai chi or had seen a massage therapist or chiropractor said it had helped them. That amounts to nothing more than an uncontrolled collection of testimonials. It’s not science.
They quote an integrative medicine specialist who says conventional treatment fails because it doesn’t treat the whole patient. But they offer no evidence that an integrative medicine approach gets any better results.
They quote Nitin Damle, a former ACP president: “Many physicians who are used to writing prescriptions right off the bat or sending patients for tests are going to have to rethink the way they manage back pain.” They say 82% of their survey respondents reported getting an X-ray, CT scan, or MRI. And 57% were prescribed opioids. And three-quarters of them tried bed rest. I find it hard to believe that represents common practice. It certainly doesn’t fit with published evidence-based recommendations.
In my opinion, they grossly mischaracterize conventional care. The practices they describe may be true of some substandard doctors, but good evidence-based doctors shouldn’t be doing those things.
The evidence-based standard of care
According to an evidence-based review article in American Family Physician, the journal of the American Academy of Family Physicians:
- Imaging with x-rays, CTs, or MRIs is not warranted unless there are red flags.
- Bedrest should be avoided.
- Adding chiropractic techniques to established medical treatments does not improve outcomes.
- Acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDS), and muscle relaxants are somewhat effective.
- Opioids are strongly discouraged. “Opioids are commonly prescribed for patients with severe acute low back pain; however, there is little evidence of benefit.” They cite three studies, and they point out the risks associated with opioids.
- Physical therapy, ice, and heat treatments are supported by evidence.
- No substantial benefit has been shown with oral steroids, acupuncture, massage, traction, lumbar supports, or regular exercise programs
The second article: Patient reports of what was helpful
In another article, they report treatments listed in order of how well patients in their survey thought they worked: yoga and tai chi topped the list, followed by massage, spinal manipulation, physical therapy, and acupuncture. When they asked those who had consulted a professional “Whose treatments or advice were helpful?” here’s how patients answered:
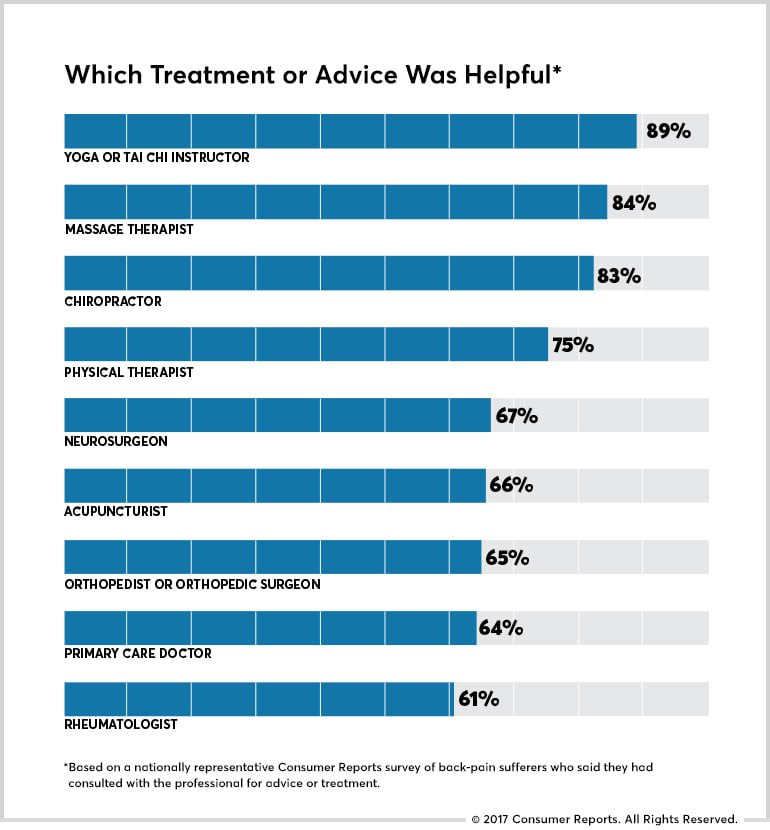
The title should have been “Which Treatment or Advice Patients Thought Was Helpful.” Deciding which treatments are effective isn’t a matter of a popularity contest or a collection of uncontrolled anecdotal reports from satisfied patients. The only way to know whether a treatment is effective is to do controlled studies.
The third article: home remedies
In a third article they cover home remedies:
Back-pain sufferers are admittedly desperate and willing to try anything—shoe inserts, devices that zap them with electric pulses, or braces to wrap around their lower back. And sales of back creams, patches, and wraps amounted to nearly $1 billion last year.
They quote a professor of rehabilitation medicine who says many of these items are expensive and research doesn’t always show that they work, and they say the ACP guidelines only found good evidence for heating pads. Nevertheless, they go on to evaluate various products and designate several of them as “Worth a Try,” and only two (At-home TENS units and insoles) as “Mostly Skippable.” Then they provide more anecdotal evidence in the form of this table:
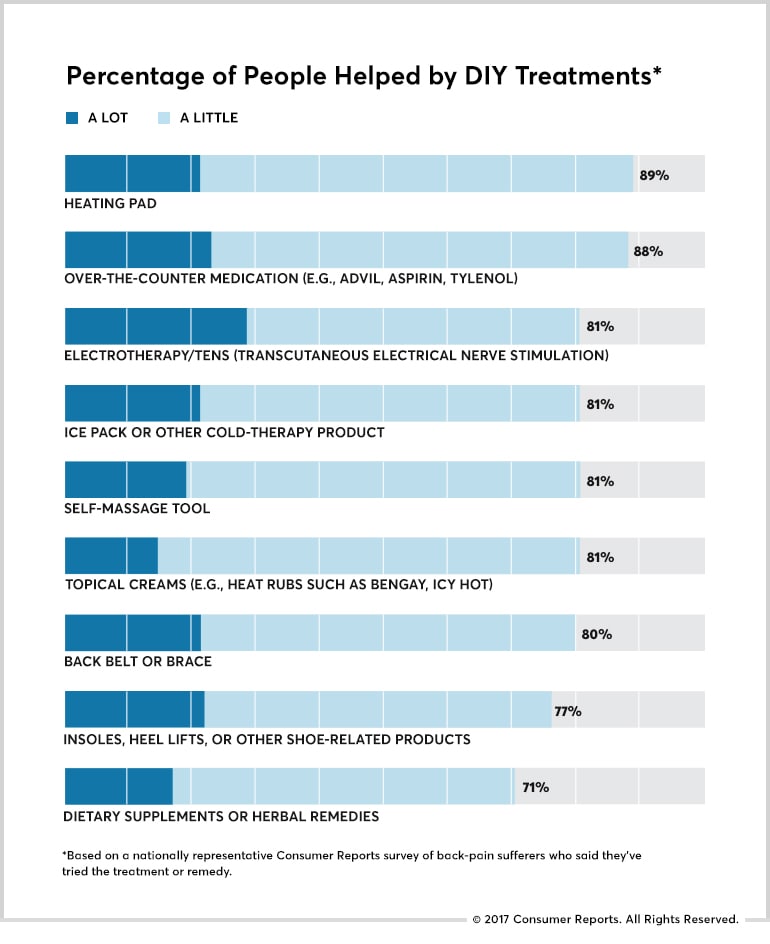
The title should have been “Percentage of People Who Thought They Were Helped.” Back pain is usually a self-limiting condition that will improve on its own even if no treatments are used. People who thought they were helped had no way of knowing whether the treatment was responsible for their improvement or whether they were fooled by a “post hoc ergo propter hoc” illusion. They got better after treatment, but did they get better because of the treatment? A man I know phoned a chiropractor’s office on Friday and made an appointment for Monday. On Saturday, his back pain went away, never to return. If he had seen the chiropractor on Friday, the chiropractor would have falsely gotten the credit for his recovery. Surveys like this without a control group are meaningless.
Consumer Reports quality varies
It’s not all bad. A new article in Consumer Reports reliably reports valuable information about a medical treatment. It’s the sort of thing I would have expected from them. It describes an analysis of 28 brands of red yeast rice supplements. The active ingredient in red yeast rice is monacolin K, the same cholesterol-lowering statin compound found in the prescription statin drug Lovastatin. They found varying quantities of the active ingredient: two brands contained none at all, others ranged from negligible amounts to concentrations higher than the amount in prescription pills. The labels were inaccurate. The manufacturers failed to warn about taking it in conjunction with prescription drugs, and they didn’t warn about the side effects of statins. Some red yeast rice supplements also contain a toxin, citrinin, which might cause kidney failure. The FDA warns manufacturers that if their product does contain therapeutic doses of monacolin K, it qualifies as a drug and can’t be marketed as a supplement.
I used to consult Consumer Reports for what I thought were reliable facts about appliances and cars. I wanted to know which cars got the best mileage and required the fewest repairs, not which ones were judged most stylish and sexy in a popularity contest. I wanted to know how one brand of appliance performed compared to other brands, not which brand people said they enjoyed using or thought was more pleasant to look at.
Conclusion: Not what I wanted to know
I found the articles on back pain very disappointing. I hope I can still trust Consumer Reports when shopping for a washing machine, but I have no confidence that I can trust them when looking for an effective medical treatment. They seem not to understand the difference between anecdotes and data, between a popularity contest and a controlled scientific study. These articles may do harm by encouraging readers to try treatments that don’t work and by suggesting that it is reasonable to prioritize testimonial evidence over scientific studies. On the other hand, these articles may do some good insofar as they may dissuade some patients from rushing to a doctor and demanding imaging studies or prescription drugs.
One thing I wish they had mentioned is the option of toughing it out with no treatment and staying as active as possible. That’s what I did when I had a bad episode of low back pain, and it was gone in about ten days. In most cases low back pain will resolve with “Tincture of Time,” which costs nothing and has no side effects.
