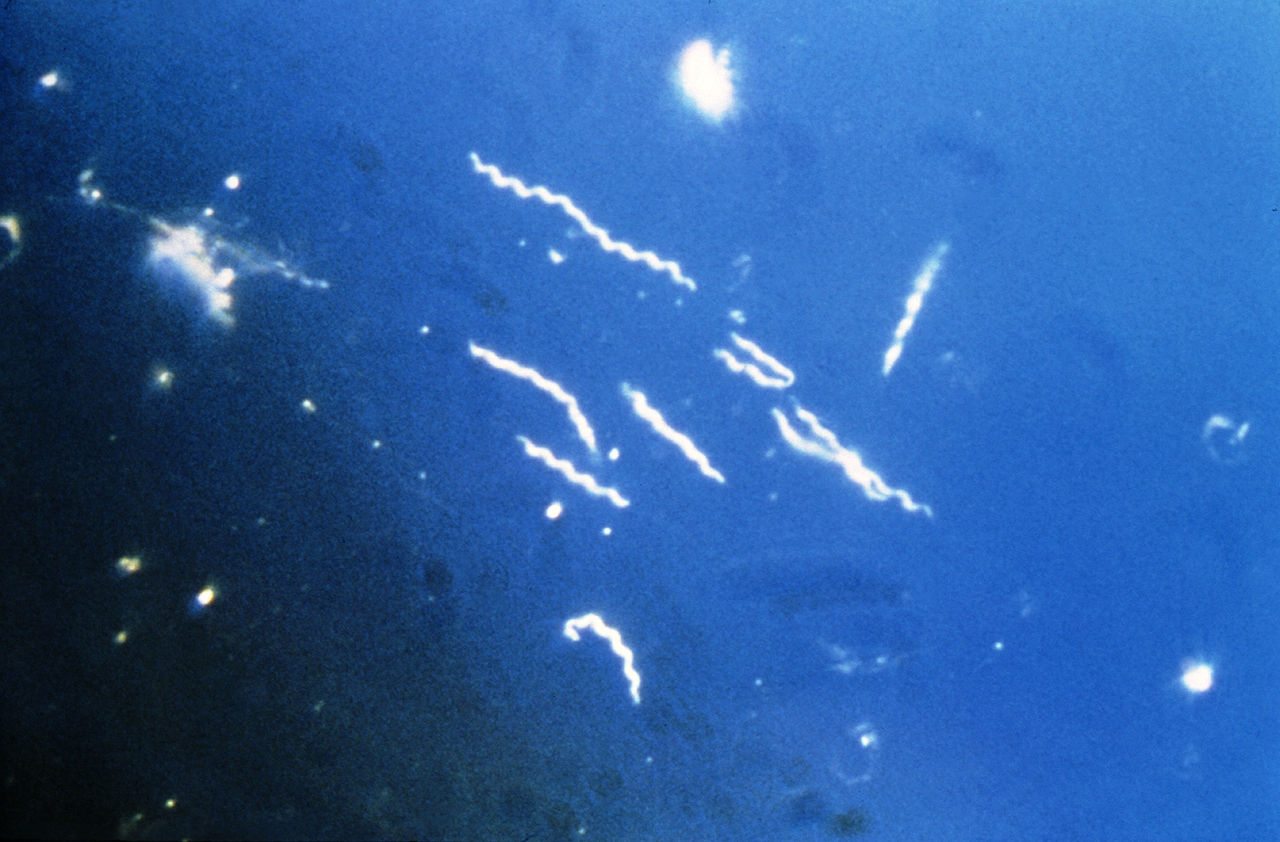
Borrelia burgdorferi, the spirochete bacteria that causes Lyme disease.
While Lyme disease itself is a real and often serious infectious illness, the existence and proper treatment of so-called chronic Lyme disease is dubious, and some would say controversial. However, like many controversies we cover, the science itself is not very controversial, but the topic is made so by a persistent minority of outliers who refuse to accept the scientific consensus.
The issue has been raised yet again by a study published recently in The New England Journal of Medicine: “Randomized Trial of Longer-Term Therapy for Symptoms Attributed to Lyme Disease.” The study was negative, but I will get into the details below.
Lyme disease
Lyme is an infection caused by the bacteria Borrelia burgdorferi, and related species. In Europe the infecting species are B. afzelii and B. garinii. These bacteria are spirochetes, which refers to their spiral shape. They are related to the bacterium which causes syphilis, Treponema pallidum, which is also a spirochete.
Syphilis and Lyme both have three stages of illness – a primary infection, secondary symptoms, and then a persistent tertiary syndrome. With Lyme disease, stage 1 involves local infection, including headache, fever, chills, and local arthritis. Stage 2 is disseminated Lyme, including the classic target- or bullseye-shaped rash at the site of the bite, pain, weakness, fatigue, and diffuse arthritis. Stage 3 is persistent late stage infection, and includes ongoing stage 2 symptoms, heart involvement, and neurological involvement.
As you might suspect, treating the infection early is important and most effective. The bacterium is sensitive to a number of antibiotics. Doxycycline is an oral antibiotic most often given in the early stages. Tertiary Lyme often requires IV antibiotics.
Lyme can be diagnosed by a combination of presenting with the classic clinical features, and a positive antibody titer, which can be confirmed with a western blot test. Antibodies can show an acute infection, or can have a profile that reflects a past infection.
Chronic Lyme disease
Fortunately, most patients will recover from Lyme disease after an appropriate course of antibiotics. The evidence shows that antibiotics are capable of eradicating the infection, and there is no evidence that the spirochete can evade treatment by hiding out somewhere in the body, going dormant, or resisting the antibiotics.
However, 10-20% of patients diagnosed and treated for Lyme disease will continue to have chronic symptoms of fatigue, muscle aches, poor sleep, and cognitive fog. Experts believe in some cases this may be due to a post-Lyme syndrome – the effects of inflammation or perhaps an activation of the immune system. There is also the possibility that symptoms in some cases are not due to the infection itself but to another cause, which may or may not have been triggered by the infection. Possibilities include disturbed sleep, deconditioning, and depression.
There are also patients who never had confirmed Lyme disease but have a similar syndrome of pain, fatigue, poor sleep, and mental fog.
This is where the controversy comes in – there are some patients and practitioners (who sometimes call themselves “Lyme literate MDs”) who believe that these chronic symptoms are due to persistent infection with the Lyme bacteria, and that the proper treatment is recurrent and long term treatments with antibiotics, often intravenous (IV).
Their only real source of evidence for this claim is the apparent response of such patients to courses of antibiotics, and the only real published evidence is case reports and case series or uncontrolled studies. However, responses are subjective and temporary, and often patients require ongoing treatment. This has all the hallmarks of a placebo response.
Physicians and scientists skeptical of this claim (myself included) will point to the fact that patients with alleged chronic Lyme disease are often seronegative (they don’t have antibodies, or their antibodies reflect only past infection), and often lack classic clinical features of Lyme disease.
In other words, chronic Lyme advocates are claiming that their patients have seronegative, atypical, treatment-resistant Lyme disease. That is a lot of special pleading, very much like Sagan’s invisible, floating, heatless, noncorporeal dragon. The more parsimonious interpretation is that these patients do not have Lyme disease.
This is a critical distinction for two reasons. The first is that treatment with antibiotics, especially IV antibiotics, is not benign. There is tremendous potential for complications.
The second is that these patients, if they don’t have chronic Lyme disease, have something else which is being missed because they and their practitioner are distracted by the false diagnosis. This is a missed opportunity to treat the real cause of their symptoms. If there is no treatable cause, it is then better to focus on symptom management and quality of life, rather than chase a fictitious infection.
Treatment trials
Initial research trying to settle the question of whether or not chronic Lyme disease is a real entity focused on trying to find evidence for persistence of the spirochete in patients with symptoms diagnosed as chronic Lyme. Such efforts failed, but did not settle the controversy. Proponents of chronic Lyme just special-pleaded away this negative evidence.
Research efforts then shifted to seeing if such patient responded to courses of antibiotics, with double-blind placebo controlled trials. This is often a good strategy to addressing such questions, because it cuts right to the clinical management question – do these patients benefit from courses of antibiotics?
A 2013 systematic review of the major clinical trials of antibiotic use for patients with alleged chronic Lyme disease concluded:
On the basis of this analysis, the conclusion that there is a meaningful clinical benefit to be gained from retreatment of such patients with parenteral antibiotic therapy cannot be justified.
A 2015 review also concluded:
Prolonged courses of antibiotics neither prevent nor ameliorate these symptoms and are associated with considerable harm.
This brings us to the current study. I found the trial design to be a little unusual, but was justified as trying to replicate how chronic Lyme is often treated in real practice. The study occurred in Europe, and therefore involved the European Borrelia species which causes a slightly different clinical picture than the North American variant.
Enrolled patients did not need to have confirmed prior Lyme disease, so they could include both subjects with post-Lyme symptoms and subjects who never had Lyme. All subjects were given a course of IV antibiotics, ceftriaxone, for two weeks, followed by either placebo or a longer course of oral antibiotics (doxycycline and clarithromycin with hydroxychloroquine.)
The study showed no difference between the treatment and placebo groups, demonstrating that long term antibiotics are ineffective.
In an accompanying editorial, experts who were not part of the study concluded:
Critics may rightly say that this trial does not truly capture with certainty the consequences of bona fide Lyme disease. However, studies with more stringent inclusion criteria have already been conducted, and the approach used by Berende and colleagues probably reflects the common practice in ambulatory care settings, in which patient presentations of fatigue or nonspecific pain prompt serologic checks for Lyme disease, despite evidence suggesting that these tests will not identify a probable cause or result in a treatment benefit.
Conclusion: Where are we now?
If you look at the totality of scientific evidence, it does not support the existence of chronic Lyme disease or the approach of treating patients with long term or recurrent courses of antibiotics.
Patients who end up with this diagnosis tend to have non-specific symptoms that could have many causes, and lack a clinical picture specific to Lyme. They also lack serological proof of active Lyme (although may have had past Lyme). Most significantly, they do not respond to antibiotics in rigorous clinical trials.
Proponents of chronic Lyme essentially just dismiss the scientific evidence, and instead resort to anecdotal evidence of a subjective response to treatment in some patients.
As would be expected, when a group has a persistent belief that experts reject due to lack of scientific evidence, or even evidence of lack of efficacy, conspiracy theories proliferate. In this case the usual “Big Pharma” conspiracy won’t work, because the treatment being offered is pharmaceuticals. So a new enemy was invented, insurance companies. They were made the bogeyman for not wanting to pay for multiple courses of IV antibiotics.
The Infectious Disease Society of America (IDSA), a professional organization of experts who reject the claims made for chronic Lyme (and have been sued for holding that opinion), are also accused of being in on the conspiracy. What possible motive would an infectious disease society have for denying that a common illness is caused by an infectious illness?
This just shows how versatile conspiracy theories are. Villains and motives can be made up as needed out of whole cloth, without any burden of logic or consistency.
Unfortunately, gullible (or perhaps cynical) legislators have fallen for the conspiracy theory. In 2009, for example, my own state of Connecticut passed a law shielding health care providers who treat chronic Lyme with long term antibiotics from being held to any standard of care. Insurance companies and the IDSA were specifically pointed to as perpetrating a conspiracy against such providers.
At the time I argued that it is a folly for legislators to decide on what the standard of care is, let alone enshrine it into law. The standard of care is a moving target that shifts with the scientific evidence. Here we are, 7 years later, and the scientific evidence has only moved more in the direction of rejecting chronic antibiotic treatment for alleged chronic Lyme. There is no lobby, however, to get CT legislators to reconsider their past mistakes on this issue – which is precisely why you shouldn’t calcify a particular practice into law.

