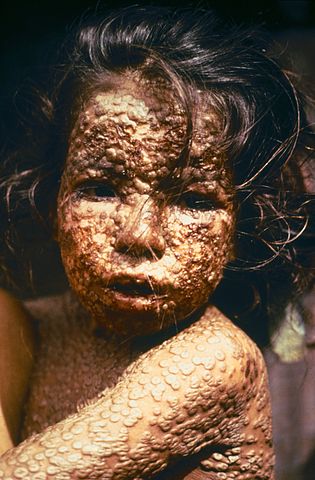
A child with smallpox; the cost of unscientific medicine. This is why science-based medicine matters.
The regular contributors at Science-Based Medicine (SBM) work diligently every week to explore the world of science-based medicine and the gauzy, nebulous netherworld of fantasy-based medicine. They shine light on the leading edge of medical science, dissect the nuances of mainstream care, expose the misconceptions and sometimes the frank deceptions of so-called alternative medicine. Launching SBM on January 1, 2008, sbmadmin (Steven Novella?) described the mission of the blog as: “scientifically examin[ing] medical and health topics of interest to the public [including] reviewing newly published studies, examining dubious products and claims, providing much needed scientific balance to the often credulous health reporting, and exploring issues related to the regulation of scientific quality in medicine.” He went on to propound an elegant yet simple core philosophy that “safe and effective health care is critical to everyone’s quality of life; so much so that it is generally considered a basic human right.”
This last deserves, I think, especially careful consideration. Enshrined in the aspirational manifesto of the United States, the Declaration of Independence, is the claim for all people to inherent and inalienable rights to “Life, Liberty and the pursuit of Happiness.” And while Jefferson used the phrase in the context of personal political freedoms, health is central to the exercise of those rights. It is the role of medicine to secure health, to provide a structure and a system by which all can live life as long and as free from disease and disability as our individual circumstances allow.
What came before
Our efforts to formalize the management of human health date back long before Hippocrates and, several centuries after him, Claudius Galen who codified the sum of what then passed for medical knowledge in the West. Ayurveda claims a history of 5,000 years, Traditional Chinese Medicine at least 2,500 years, and other cultures from Babylon to Egypt had medical traditions of varying degrees of formalization. But these were medicines of speculation, of humours and miasmas, of herbs and poultices, of pakrutis and meridians and qi. What is remarkable is how little these traditional medicines changed over the centuries. It isn’t that medicine was static for several thousand years, but change was incremental, stifled by unchanging conceptual paradigms, and boxed in by cultural and religious mores. For instance it wasn’t until the 13th century that an Arab physician named Ibn al-Nafis discovered that blood moved from one side of the heart to the other, first traveling through the lungs to be “mixed with air.” This overturned the Galenic belief of a porous cardiac septum, a belief held since the 2nd century.
Centuries of fits and starts of incremental progress did little to curb the major causes of morbidity and mortality. Roman babies died of pertussis when Julius Caesar declared himself emperor. Chinese babies died of pertussis in the 7th century. North American babies still died of pertussis in the early 20th century. For that matter, American babies are still dying today. In fact, this might be a good point at which to mention that it is the very young who historically have paid the steepest price for ingrained and refractory medical ignorance.
We often cite changes in life expectancy as a measure of medical progress. But as we shall see, that is a remarkably crude measure. Selected males born before 100 BCE lived a median span of 72 years , not remarkably different from lifespans in industrialized nations today. But it is important to note that the data included only males who lived long enough to make a contribution of sufficient significance that their vital data was recorded in the Oxford Classical Dictionary. Looking at changes in life expectancy for women aged 15 and older reveals a very different picture. In the 16th century these women had a life expectancy of about 48 years. Much of that premature death owed to maternal perinatal mortality. It is an interesting historical side note that it was puerperal fever (“childbed fever”), a frequent cause of maternal death, that led Ignaz Semmelweis to his work on antiseptic hand washing – part of the cascade of discoveries that gave birth to the germ theory of disease.
Pity the child
Before one can conceive or for that matter father a child, before one can make a contribution worthy of history’s notice, one must generally survive childhood. Until very recently, that was in no manner a certainty. It is very difficult to find meaningful numbers for infant mortality rates in 700 BCE China or 100 CE Rome or 800 CE Arabia. There are a variety of numbers bandied about but in the 17th century the consensus seems to be that about 30% of English children died before the age of 15, mostly from infectious diseases. Factoring in the ghastly premature deaths of children and mothers, average life expectancy in the time of the Roman Empire was perhaps 35 years. As late as 1900 in the US, life expectancy at birth for males was 46.3 years and 48.3 years for females. But if you lived to see your 20th birthday your life expectancy (white males) was 62.2 and (white females) 63.8. So when you read statistics of life expectancy in the days before modern medicine, remember that those short spans didn’t so much reflect a truncated dotage as a failure to survive childhood – or even the miracle of childbirth.
Rubella, measles, diphtheria, smallpox, puerperal fever, the odd plague, scarlet fever, pneumonia, tuberculosis, and a host of other diseases thinned the herd of infants and children. And whether in China or Africa or Asia or Europe, traditional medicine treated these diseases with herbs and needles and spells and prayers. And thank goodness! Because with all of those “interventions” only about 30% of children died. Of course only about 30% would have died without the interventions. And given some of those treatments – bleeding comes first to mind – perhaps doing nothing might have yielded slightly better mortality rates.
But in the eyes of the times, recoveries were miracles of what then passed for medicine. Chen Liu was ill. The traditional healer came. After some days, Chen Liu was better. Give thanks to the traditional healer! This is a classic example of confusing correlation with causation. The human body maintains a wide variety of parameters within very narrow limits: core temperature, blood pH, partial pressures of oxygen and CO2, and very many others. The balance achieved is referred to as homeostasis. When one or more of these parameters drift out of normal range, various biological processes work to restore homeostasis. When disease or injury disrupts homeostasis, one of two things happens: either homeostasis is eventually restored and you get better (sometimes referred to as regression to the mean) or you die. The mechanisms that directly and indirectly enforce homeostasis are very powerful indeed, so regression to the mean is, generally speaking, the usual outcome. But with disease or injury there is often uncertainty. So when a shaman or healer intervenes and the patient recovers, it is easy to credit the intervention. And when the patient dies it is because the shaman wasn’t summoned soon enough.
Belief is powerful, yet powerless
And so it goes. Or so it went. Disease was caused by unbalanced humours, miasmas, disrupted qi, evil spirits, or whatever you did to piss off the gods. Healers responded with the tools they had. They poked needles to unblock qi, they bled patients to balance humours, they prayed to the offended gods, they applied poultices and prescribed herbs. The common thread is that all of these approaches were based on beliefs rather than knowledge, and those beliefs were absolutely, flatly wrong*.
Belief is a powerful thing – and all too often an easy thing. The beliefs of our forebears are often unquestioned and comfortable. The first effort to conceptually challenge blind faith in received wisdom was perhaps taken by Thales of Miletus, a 7th century BCE Ionian philosopher who worked to understand the world in natural terms without relying on mythology or supernatural explanations. Reason and rationality again flourished for a time during the Islamic Golden Age with significant contributions to mathematics and astronomy and, as mentioned earlier, even medicine. There were brilliant insights and discoveries throughout these long centuries, but they were, by and large, naked flashes against a dark fog of long cherished beliefs, unquestioned religious dogmas, and primeval superstitions. What there wasn’t, was science, at least not in the sense of a broadly organized effort to understand reality.
Beliefs die a hard death. By way of illustration, On the Origin of Species was published in 1859. The Scopes “Monkey” trial was held in 1925. The US Supreme Court ruled against teaching Creationism in Edwards v. Aguillard in 1987. Over the years an imposing body of evidence supporting evolutionary theory has been assembled. Yet still in 2016, long past Origin’s sesquicentennial, groups such as The Discovery Institute still peddle a version of creationism they style as “Intelligent Design.” Despite the overwhelming mass of evidence supporting evolution, despite virtual unanimity of scientific consensus, a Gallup poll in 2014 found that 42% of Americans believe that “God created humans in present form.” Another 31% allowed that humans evolved, but with God’s guiding hand. Only 19% understood that humans evolved through natural processes and without necessity of supernatural intervention.
The fog of dogma and superstition began to lift as the Enlightenment rolled across Europe in the 18th century. Blind faith – in religion, in monarchies, in hidebound beliefs long sheltered from doubt – was shaken by a new willingness, a new impulse to question and reexamine. By the 19th century the millennial shackles of medical thought began to crumble as Schwann and Schleiden described their theory of the cellular nature of living tissue, Jenner introduced smallpox vaccination, Lister built on the work of Pasteur by introducing antisepsis in the form of carbolic acid to sterilize surgical instruments and surgeons’ hands. It was clear that the medicine of Galen, a medical tradition that had endured for well over one thousand years, was crumbling.
The inevitable backlash to reason
But then, as now, logic and reason are not everyone’s cup of tea. The profound challenges unleashed by the Enlightenment also triggered the Romantic backlash of the 19th century and with it renewed interest in vitalism and, especially in North America, spiritualism and religiosity. Mormons, Seventh Day Adventists, Jehovah’s Witnesses, Christian Science, and other religions sprang to life. And efforts to fill the void of the rapidly collapsing Galenic tradition were not limited to scientists.
Samuel Hahnemann propounded homeopathy around 1800. Hahnemann, a medical doctor from what is now Germany, was troubled by the increasingly obvious flaws of Galenic medicine. He recognized that the treatments he learned in medical school often seemed to do more harm than good and he quit the practice of medicine within a few years, earning his living as a translator and writer. While translating Cullen’s A Treatise of the Materia Medica Hahnemann encountered the claim that the bark of the South American cinchona (Cinchona officianalis) was an effective treatment for malaria because it was a bitter astringent. Hahnemann doubted that astringency alone accounted for cinchona’s effectiveness, questioning why any other astringent wouldn’t have the same effect. Hahnemann, though not suffering from malaria, decided to experiment with cinchona on himself and found that ingesting some the material produced symptoms which he imagined to be malaria-like. From this he extrapolated the dogma of “that which can produce a set of symptoms in a healthy individual, can treat a sick individual who is manifesting a similar set of symptoms.” This is the “like cures like” principle on which homeopathy is based. This massive leap of intuition was, and remains, spectacularly wrong.
You will note the ‘sciencish’ impulses that lie within Hahnemann’s journey. He recognized serious problems with Galenic medicine as it was practiced in his time, he questioned an understanding of a then mainstream treatment for a serious disease, and he attempted, albeit ineptly, to do an experiment to improve his understanding of that treatment. Unfortunately, the whole enterprise was built on the fantasy that it was the astringency of the cinchona bark and its “tonic effects on the stomach” that gave it therapeutic efficacy. We now know that cinchona bark contains quinine among a variety of other compounds not all of which are benign. In the event, what Hahnemann constructed was nothing more than a classic argument from false premises – and he attempted to build an entire medical paradigm around it.
Flexner and the founding of American scientific medicine
Hahnemann was not alone among 19th century medics to behold the many shortcomings of medicine and to propose a new approach. Near the end of that century DD Palmer proposed chiropractic (and for a time considered establishing it as a religion) and Benjamin Lust founded the panvitalist cesspool of naturopathy. All were creative and not one was scientific in any meaningful sense of the word. Each replaced one set of fantasies with another. Physicians of that era gleefully picked and chose from that cornucopia of delusion to practice as they best saw fit. The practice of medicine grew more diverse but precious little grew better. By 1904, the American Medical Association had had enough and established the Council on Medical Education to bring some order to the chaos. In furtherance of better medical care, the Carnegie Foundation, supported by the AMA, commissioned Abraham Flexner to study medical education in the United States and Canada. The resulting Flexner Report [PDF] eviscerated medical education as it then existed in North America and resulted in the closing of a large portion of the medical schools then operating. Flexner was himself not a doctor, but would probably today be recognized as an expert in pedagogy. Why a pedagogue you ask? As Thomas Duffy notes:
Flexner was an unorthodox and surprising candidate for the task he was asked to undertake. Flexner himself was quizzical about the summoning, suspecting that he was being confused with his brother, Simon. At the time of the job offering, the former high school teacher had never been in a medical school. This shortcoming might have seemed an insurmountable impediment for successful performance of his assigned task, but the choice of a non-physician was purposeful on the part of Pritchett and his associates. They perceived the problem of medical education as a problem of education and believed a professional educator was better qualified to address this dimension of the problem. They also had preconceived ideas concerning what changes needed to be made in medical schools to allow these ideas to be introduced. The ideas Flexner popularized were those that had already been developed within medical schools before the turn of the century. Pritchett (Henry Smith Pritchett was president of the Carnegie Foundation from 1906-1930) and colleagues also were concerned that antagonisms would be generated by the report, which might be less vengeful if a non-physician were the object of the resentments. An unflattering but not necessarily inaccurate description for Flexner’s assignment was that he was to be the hatchet man in sweeping clean the medical system of substandard medical schools that were flooding the nation with poorly trained physicians.**
Flexner and his Report, of course, did not change medical education single-handedly; his contribution should not be oversold. In important ways he was simply a reporter of facts – and often a lightning rod. Giants including William Osler and William Welch (two of the four founders of Johns Hopkins Hospital) shaped the contours of what would become modern medical education. But neither should Flexner’s role be undervalued. He laid bare a medical education system that was outdated, inconsistent, and mostly ineffective. And he promoted the “German System of Medical Education” and its program in which “physician scientists were trained in laboratory investigation as a prelude and foundation for clinical training.” This was the seed from which modern medicine, science-based medicine, took root.
Before Flexner, medicine had changed only incrementally since the time of Galen – the better part of 2,000 years. In the hundred years since Flexner, medicine has been radically transformed and with it the human condition, from the Hobbesian “nasty, brutish, and short” to a span rapidly closing on nine decades of often quite good health. While homeopaths shook their little vials of magic water, science-based medicine eradicated smallpox, a disease that as recently as 1948 infected 50 million people worldwide. Chiropractors imagined subluxations were the one true cause of all “dis-ease.” They adjusted and twisted and prodded while science-based medicine learned to type and transfuse blood and conquered, for instance, most childhood leukemias. Naturopaths flushed pounds of imaginary ‘toxins’ from colons, while science-based medicine identified the virus that leads to AIDS and developed Highly Active Anti-Retroviral Therapy to manage the disease.
The turning point: A method, not a fact
The inflection point on which this revolution turned was not a powerful new type of microscope or a brilliant new surgical technique or a dramatic insight into how some organ system worked. It was a change in the manner of thinking. No longer would intuition and belief and the received wisdom of our forebears be enough. Henceforth these would be hung, along with new insights and developments, on the cold rack of the scientific method and rigorously tested. This was the moment when the paths of medicine and the array of fantasies and delusions that now self-identify as “integrative medicine” parted. Medicine’s commitment to science led to the cascade of advances in understanding and application that today render obesity a far bigger concern to most people than, say, diphtheria.
Science works. It delivers the goods. In 1900 the top causes of death were pneumonia, tuberculosis, and diarrhea and enteritis. Today, accidental injury claims more lives than any of them. In 1969 the age-standardized death rate from heart disease was 520.4 per 100,000. By 2013 the mortality rate was less than half that: 169.1 per 100,000. This was not by happy accident. This was not the result of deeper understanding of chiropractic subluxations or new insights into the vital force. It was the result of the hard work of thousands of research scientists and physicians painstakingly peeling back layers of ignorance and illuminating the innermost workings of biology and disease.
The cost of medicine without science
This is not to say that quacks do not try to wrap themselves in the trappings of science. Journals of rank silliness litter the professional literature. Schools of naturopathy teach courses in microbiology and immunology. Homeopaths jabber about the quantum nature of water memory. This is not science, it is cargo cultism. The philosophical underpinning of medicine is science. The philosophical underpinnings of ‘alternatives’ to medicine are alternatives to science: vitalism, spiritualism, superstition. And let no one forget that the sum of the contributions of naturopaths, of chiropractors, of homeopaths and the rest of the alternative practitioners to the revolution in health care has been and remains … zero. Not one insight, not one discovery that has meaningfully changed the face of health care.
Imagine for a moment that Flexner and Welch and Osler had occupied themselves with astronomy or law rather than to medicine. Imagine life today with medical care delivered by homeopaths and naturopaths and chiropractors and reiki “masters”. Imagine a health care paradigm that rejects vaccinations. Smallpox would likely continue to ravage the developing world and pertussis infections could still kill ten thousand children each year. Imagine a health care paradigm that holds human health to be regulated by qi or by the ‘vital force’ revered by naturopathy. Childhood leukemias would still be death sentences. Liver disease would be treated with spinal adjustments and diabetes treated with colonics and macrobiotic rice. In short, imagine that alternative medicine is the only medicine we have. That was largely the reality until medicine chose the arduous path of science over the easy embrace of custom and convention.
That is why science-based medicine matters. Medicine without science is the medicine of Galen. It is the medicine of bleedings and herbs and colonics and prayer. Science-based medicine is the germ theory of disease, it is antibiotics and antivirals, it is kidney dialysis and cardiac pacemakers. Science is the flashlight that reveals the wires and the gears and the pushrods of human biology. Alternative medicine is the opposite of a flashlight. It is a flashdark that substitutes fear for knowledge, superstition for understanding, ignorance for insight.
Immanuel Kant saw enlightenment as “man’s emergence from his self-imposed childishness.”*** We stand today in witness of a revolution in our understanding of biology. We have exposed the workings of the very recipe of life and are rapidly learning the often-interconnected functions of various genes, the implications of this and that allele, the secret lives of some proteins. We are building the tools to reshape malfunctioning genes, viruses to carry new instructions to cellular machinery, systems to build entire new organs.
When I was a child, I spoke as a child, I understood as a child, I thought as a child; but when I became a man, I put away childish things. For now we see in a mirror, dimly, but soon face to face. Now I know in part, but soon I shall know just as I also am known. Corinthians 13:11. Kinda
It is past time for us to put aside our childish things. A future of better health and happier lives lies in our deepening understanding of our biology. This understanding will be found in electrophoresis gels and chromatograms and the tireless work of thousands of scientists and physicians, not in color flecks in irises or the memories of water molecules.
Notes
*Of all this nonsense, sometimes the herbs had actual biological effects and sometimes those effects were even useful in treating the disease the patient actually had. But diagnosis was imprecise and the dosage of herbs less precise still. The marrying of effective dosage of herb and disease for which it was appropriate was largely a matter of serendipity.
** I would like to acknowledge that regular SBM commenter and moderator William Lawrence Utridge drew my attention to some of the controversy surrounding the Flexner Report.
*** Kant uses the word ‘Unmündigkeit’ which has been most often translated as ‘nonage’ or ‘immaturity.’ I argue that the word ‘childishness’ more fully conveys Kant’s intent.
