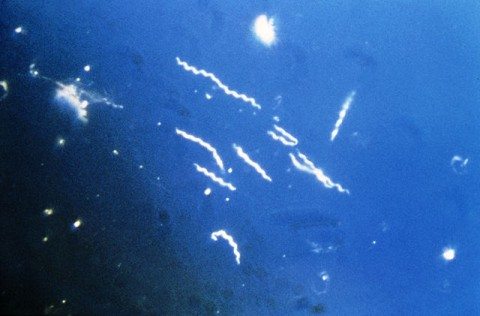
The little burrowing bacteria that bores into your pores to cause Lyme disease, EEEEEWWW!!! Darkfield 400x microscopy image of the 10-25µm long Borrelia burgdorferi spirochaete which causes Lyme disease (1993). Provided by the CDC’s Public Health Image Library (PHIL #6631) via the Wikimedia Commons
I hate those oh hell moments. I was up way too late last night, but who can pass up the opportunity to see Patti Smith playing Horses (and more) for the 40th anniversary of the album. Only 44? Behind the Eagles? No way. I would nudge it up a few more spaces. Hard to believe I was 18 when that album came out. Horses is one of the few albums that made the transition from vinyl to CD. It was a tremendous show, and at 69 Patt performs with the energy and passion of a 29 year old. And she sure can spit. I had the evening off, so food and drinks at Swine until well past midnight. First time my wife and I closed a bar. I am too old for this.
But as I was blearily drinking my a.m. coffee on a dreary PDX morning, I opened the browser to SBM and there was a post by Jann. Oh hell. That means I have a post due tomorrow and I had lost track of the time over the holidays. I thought my next post was next Friday. Oh. Hell. So unlike most posts which I write over a week, this one was done in about 4 hours. And I am sure it will show.
How do you diagnose an infection?
Not always so simple. You always start with a history and, for infectious diseases, an exposure history is paramount. People get what they are exposed to, so you want to know travel, animals, diet, water, sex etc. If you have ridden a horse to have sex in an Indian lake while drinking raw milk (not really an unusual history in my practice; people do the darndest things) you have exposure risks for a variety of infections. If you have not left the Willamette Valley it is unlikely that the cause of the illness is malaria, although you always have to consider that the infection came to the patient rather than the other way around.
A panoply of bacteria
In Oregon it is also unlikely that the cause of your symptoms is Lyme, as we do not have much Borrelia in the state. Yet there are many symptomatic people who have a positive blood test for Lyme. Having a positive blood test for a disease is a very powerful confirmation that you have a disease, right? Well, yes and no. Like much of medicine, it is not as straight forward as one would like.
First, Borellia. In the US, Lyme is due to Borrelia burgdorferi. In Europe there are Borrelia burgdorferi, Borrelia afzelii, and Borrelia garinii. And there are the relapsing fever Borrelia, B. recurrentis, B. hermsii, B. parkeri, or B. miyamotoi, the last probably more common than suspected. And there are other spirochetes, like syphilis and leptospirosis, in family. Spirochetes are a large phylum of what I think are particularly evil appearing organisms. They just look pathogenic and I can always imagine them corkscrewing into tissues to cause disease.
The gold standard in ID for diagnosis is culture. If you can grow the organism then you have the diagnosis. Usually. Again it depends. The world is a remarkably filthy place and sometimes the cultures are contaminated. And more aggravating are negative cultures. There are a variety of reasons that cultures can be negative, but the main one is that we simply cannot grow the vast majority of microorganisms from people or the environment. Some organisms, such as Borrelia, are too difficult to grow outside of specialty labs.
When you can’t grow an organism you have to rely on less accurate methods of diagnosis. Some diseases, like syphilis and extrapulmonary tuberculosis, remain very difficult to rule in or out with confidence, despite plaguing humans for millennia.
Lyme testing: Do little but dab it
For US Lyme we rely on indirect, two-step testing to determine if the disease is present; first is a screening ELISA followed by a confirmatory western blot. The test we use was validated in patients with culture-proven Lyme, so we know what the false positive and negative rates are, the sensitivity and specificity.
The ELISA is a screening test and, like many screening tests in ID, are designed to be overly sensitive. You don’t want to miss a real case of Lyme but it is at the cost of having a positive test that due to other processes. Remember all those spirochetes mentioned above? They, and other infections, can lead to a positive Lyme ELISA. The ELIZA is sensitive, but it is not specific. It will pick up Lyme, but a lot of other diseases as well.
To get a more specific answer, you do a western blot. The western blot has two flavors, the IgM (for acute disease) and the IgG (for more prolonged disease). IgM is the first antibody to respond to infection, lasting a couple of months and eventually supplanted by IgG, which is lifelong. The current testing may occasionally give a positive that is actually from infection due to B. miyamoitoi in the US, but for spirochetes, there is not a lot of data, but most will have a negative western blot.
So a positive standard two step Lyme test says you have (or had if it was treated) Lyme disease. But that is the problem with serology – it does not say if you have active disease or reinfection. That is where risk and symptoms come to play.
The diversity of species
But what about European Lyme? Is the Borrelia in Europe the same as in the US? Doubt it. Organisms separated by geography will diverge. It has happened with histoplasmosis, coccidiomycosis and Plasmodium ovale to name but a few. They may look the same and act the same but genetically they are different. The same applies to US and European Borellia; they are different enough that it affects testing. The US two-step test was developed against a US strain of Borrelia and is probably not optimal for the diagnosis of European Lyme. A better test if you can’t fly back to Germany is probably the C6 ELISA, and that may be a sufficient screening test that does not need a confirmatory Western blot.
It is an interesting question whether the genetic diversity of Borrelia as you get further away from the NE epicenter may alter the sensitivity of Lyme testing if using tests developed in the US. There are also issues in the future with genetic drift due to climate change and the movement of the animal reservoirs, the natural evolution of the organism, and the discovery of other Borrelia that could affect the epidemiology and testing for Lyme. As of now, these do not appear to be issues and the standard testing remains both sensitive and specific for diagnosing Lyme.
All this testing is under the assumption that there is a reasonable pretest probability that the patient could have Lyme. If the pretest probability is low, as in Oregon, any positive test in a patient with no risk and atypical symptoms is likely a false positive:
Predictive value is determined both by test characteristics (sensitivity and specificity) and, importantly, by the population in which it is used. The practice of testing patients with a low likelihood of Lyme disease can generate more false-positive results than true-positive results, resulting in misdiagnosis and thereby harming ill people…However, when the pretest probability is low, most positive test results are false positives (67%).
That is a tough concept for doctors and patients to wrap their heads around with any type of testing. The test is positive; it must be due to disease.
What about other Lyme tests?
With little oversight, laboratories can develop their own tests and offer them to patients. The questions are whether they are accurate, and what they were validated against, so you know what the true sensitivity and specificity is. Many of the alternative tests for Lyme have no documented validation, so their sensitivity and specificity is not known. And some labs have their own unvalidated interpretation of the standard two step. Any indirect test for infection has to be validated against a population with known disease, patients with positive cultures, to be of use.
The specialty labs for Lyme testing have been evaluated and found to be wanting, with false positive rates approaching 50% depending on the lab. With the Lyme specialty laboratories:
…one could claim that their methods provided greater sensitivity. However, this increase in sensitivity came at what can only be considered an unacceptable price, a steep decrease in specificity: 15 of 40 (37.5%) of the normal healthy controls met their IgM criteria, 11 of the 40 (27.5%) met their IgG criteria, and 23 of the 40 healthy controls (57.5%) met one or the other.
Widespread testing for Lyme in populations at little risk for the disease offers little benefit:
With 20%–25% of the population having nonspecific complaints, the positive predictive value of a positive serology using CDC criteria, IgG only for complaints of >4 weeks, is extremely poor. It is certainly not diagnostic. For serologies with specificities like those of reported for Lyme specialty laboratory B, a “positive” serology in this patient population has such a low positive predictive value that it has virtually no value. Simply stated, basing a diagnosis of LD or any other tick-borne infectious disease on the presence of ≥1 of these common vague symptoms is unjustified.
These unvalidated tests are one of the reasons why the FDA is in investigating the process by which these labs offer their tests.
And, interestingly, those with false positive Lyme serologies get labeled as chronic Lyme disease but their clinical presentation is identical to patients diagnosed with chronic fatigue syndrome (now called systemic exertion intolerance disease, abbreviated SEID). Whatever the etiology of SEID is, it is a debilitating illness and sloppy diagnostic testing will result in patients being funneled into the black hole of chronic Lyme treatment instead of, hopefully, the more fruitful future of SEID research.
Alternative tests: More “science fiction” than science
Other diagnostic tests not to be used for Lyme:
- Capture assays for antigens in urine
- Culture, immunofluorescence staining, or cell sorting of cell wall-deficient or cystic forms of B. burgdorferi
- Lymphocyte transformation tests
- Quantitative CD57 lymphocyte assays
- “Reverse western blots”
- In-house criteria for interpretation of immunoblots
- Measurements of antibodies in joint fluid (synovial fluid)
- IgM or IgG tests without a previous ELISA/EIA/IFA
And, unfortunately, the PCR is of little use.
Of course it’s really all just a conspiracy!
There does need to be better Lyme testing. As a practicing ID doctor, tests like these are an indirect means of diagnosing disease; while very good, they are still far from ideal. I am sure there will be no CDC-supported test that will satisfy those who believe in chronic Lyme disease. In that universe there are no false positive tests, only false negatives, and the CDC and FDA are in a conspiracy to cover up the truth about Lyme.
For Lyme, and many other infections, diagnosing a disease is not based on a test in isolation. It depends on the risks, the symptoms, and the operative characteristics of the test. No specific risks, no characteristic symptoms, and a positive result from an unvalidated test, is not the way to diagnose Lyme.
