In 2011, Americans spent some $30 billion on dietary supplements. Yet, except for the industry itself and a few politicians and “health freedom” advocates, you’d be hard pressed to find anyone (who’s given it some thought) of the opinion that dietary supplement regulation is adequate. Three recent reports, two from the government and one from a newspaper, demonstrate why this near-universal conclusion is warranted.
Another government report on lax supplement regulation
Here’s how an October, 2012, Department of Health and Human Services Office of Inspector General’s (OIG) report described the FDA’s regulatory authority:
DSHEA [Dietary Supplement Health and Education Act] does not require manufacturers to submit dietary supplements to FDA for safety or approval prior to sale. As a result, FDA has no comprehensive list of dietary supplements on the market. Dietary supplement manufacturers must ensure that their products are safe, they have evidence to substantiate structure/function claims, and that product labels are truthful and not misleading.
In other words, the fox guards the henhouse.
Because there is much confusion about structure/function claims, here is a somewhat lengthy explanation from the report about what they are and how they are different from disease claims, which dietary supplement manufacturers aren’t supposed to make. (Citations omitted.)
In general, structure/function claims describe the role of a dietary supplement in the structure and function of human bodies, but the claims may not explicitly or implicitly claim to prevent, treat, mitigate, cure, or diagnose a disease. A structure/function claim may also:
• claim a benefit related to a classical nutrient deficiency disease (e.g., scurvy) and disclose the prevalence of such disease in the United States,
• characterize the documented mechanism by which a nutrient or dietary ingredient acts to maintain such structure or function, or
• describe general well-being from consumption of a nutrient or dietary ingredient.
For example, a supplement may claim that it “curbs appetite to help with weight loss,” but it may not claim to “aid weight loss to treat obesity” because obesity is a disease. Similarly, a supplement may claim to “support immunity,” but may not claim to “boost the immune system against colds and flu” because the latter references specific diseases. Although FDA has issued regulations and published guidance describing the difference between structure/function claims and disease claims, it acknowledges the challenge of distinguishing between the two.
If the FDA has trouble interpreting DSHEA and its own regulations, imagine the problems everyone else has with “the challenge of distinguishing between the two.” The report continues:
DSHEA requires manufacturers to meet three requirements for placing a structure/function claim on a supplement label: (1) substantiation that the claim is truthful and not misleading, (2) notification to FDA within 30 days of marketing the supplement with the claim, and (3) a disclaimer on the supplement label.
“Substantiation of structure/function claims” means:
Manufacturers must have substantiation for the structure/function claims on their products’ labels to ensure that they are truthful and not misleading. . . .
However, this substantiation requirement is, shall we say, substantially limited by the fact that:
In any legal proceeding concerning structure/function claims, FDA must prove that the claim is false or misleading.
A further limitation is:
DSHEA does not require manufacturers to submit the substantiation requirement to FDA to determine its adequacy and FDA may not compel manufacturers to produce substantial upon request.
So, let’s see. DSHEA requires substantiation of structure/ function claims but manufacturers are under no legal obligation share that information with the FDA even if the FDA asks for it. All the manufacturer has to do is notify the FDA of the structure/function claim and slap the Quack Miranda Warning on the label. Then it’s off to market. The burden is on the FDA to identify risky supplements, of which there are about 85,000, according to a recent New York Times story. And if the FDA takes a manufacturer to court it is up to the FDA to prove the lack of substantiation. In a classic case of bureaucratic understatement, this caused the OIG to conclude that the FDA “has limited authority to enforce the substantiation requirement.” Indeed.
And how is industry doing with that substantiation?
Even with these slack requirements, a sampling of 127 supplements marketed for weight loss and “immune system support” revealed manufacturers did not fully comply with FDA guidance on proper substantiation of claims. A wide variety of brands were selected from various locations across the country and the internet. A truly random sample was not possible because “no comprehensive list of dietary supplements or manufacturers exists.” The OIG would have looked at more supplements but only 61% of the manufacturers complied with its request for information. Here’s a sampling of structure/function claims from the report:
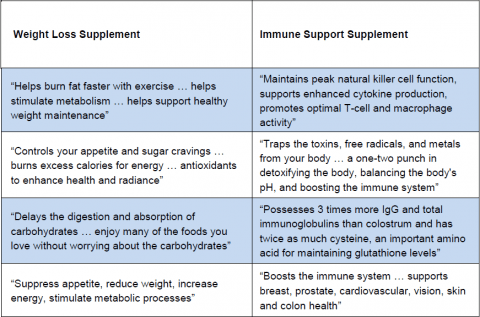
Based on its review, the OIG concluded:
- Most substantiation was not derived from human studies. 56% would be considered background information (e.g., in vitro and animal studies), which are not primary sources of evidence and therefore may not be sufficient to support claims.
- None of the human studies met all of the FDA’s recommendations for competent and reliable evidence.
- Human studies rarely showed a direct relationship to the claim. For example, evidence submitted to support a supplement claim that it burns fat because it contains a green tea extract was actually a study of drinking green tea.
- Most human studies did not appear to represent the totality of the evidence. In this conclusion, the OIG relied on NCCAM staff, who told them that a large body of evidence contradicts structure/function claims. But a whopping 96% of human studies the OIG received were favorable to the supplement’s claim.
- Most studies were not consistent with FDA guidance on quality. Another whopping figure here – 85% were not randomized, double-blind, parallel group, placebo-controlled trials.
- About a third were not consistent with FDA guidance on the meaning of the claim made.
- 10% did not qualify as substantiation at all.
As an example of this last deficiency, the OIG noted:
One company submitted a 30-year-old handwritten college term paper . . . while others included articles from trade newsletters; press releases; advertisements; and links to Web pages, such as Wikipedia or an online dictionary.
Only drugs can legally make disease claims, yet 20% of the supplements made such claims. Another chart from the study:
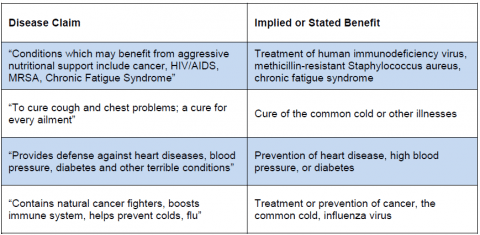
The manufacturers couldn’t even get the bonehead requirements right. A majority of notification letters were missing required information. And 7% didn’t have the Quack Miranda Warning on the label.
In response to the report, the FDA said it would improve its notification system for structure/function claims, expand market surveillance to detect disease claims and enforce inclusion of the Quack Miranda Warning. However, as to the OIG’s recommendation that the FDA seek legislation requiring approval for all structure/function claims in labeling, the FDA would only commit to considering the possibility. Small wonder, given the fact that Congress has a conniption fit every time attempts are made to beef up regulation.
In addition to this report, the OIG issued another on dietary supplement regulation at the same time. Here, the title says it all:
Dietary Supplements: Companies May Be Difficult to Locate in an Emergency
True. When the government doesn’t know what products are out there or who makes them it would indeed be difficult to find the companies under the best of circumstances, much less in an emergency.
Putting a human face on the problem
Now to a feature story from Sunday’s New York Times, which recounts the heart-breaking tale of a body-building supplement and the death of a soldier.
In June of 2011, Michael Lee Sparling, a 22-year-old Army private stationed at Fort Bliss, Texas, collapsed after running in formation for about 10 minutes in 75 degree weather. He went into cardiac arrest and died later that day. Before the exercise, he had taken the recommended dose of Jack3d (pronounced “jacked”), a supplement sold by, among others, GNC, the retail dietary supplement chain, who advertised it as producing “ultra-intense muscle-gorging strength, energy, power and endurance.” Pvt. Sparling, who by all accounts was in excellent physical condition, purchased his Jack3d at an on-base GNC store.
Pvt. Sparling’s untimely death has once again ignited criticism of lax dietary supplement regulation in the United States, a subject we have addressed many times at SBM. Now joining the chorus of calls for reform are his parents, Leanne and Michael Sparling. Last month, the Sparlings filed a wrongful death lawsuit against GNC and Jack3d’s manufacturer, USPlabs. Ms. Sparling, who still wears her son’s dog tags, told the Times:
They just think they are too big and everybody’s afraid of them. They think I will just go away. Unfortunately for them, I won’t go away.
According to the Times, DMAA (dimethylamylamine), started out as an inhaled drug for nasal congestion. Because of potential side effects – tremors, headaches and nervousness – Eli Lilly withdrew it from the market voluntarily. In 2005, it reappeared as a dietary supplement based on the disputed claim that it can be found in a geranium grown in China. This doesn’t mean that any of the DMAA on the market actually comes from this plant, but such is the logic of the DSHEA.
Last April, the FDA sent warning letters to several supplement manufacturers saying it had no evidence DMAA is a legitimate dietary ingredient and citing its risks. (Health regulators in other countries, such as Sweden and Denmark, have actually banned DMAA-containing supplements.) Heart attacks, heart failure, kidney failure and liver failure were among the health problems reported to the FDA, as well as 5 deaths. GNC responded that it was “completely opposed to this unilateral, factually and legally unfounded action by the FDA.”
The Times story said that other organizations are also taking action. The World Anti-Doping Agency and Major League Baseball have banned methylhexaneamine, which is the same thing. The military removed supplements containing DMAA from base stores, including GNC. Col. Erin P. Edgar, a command surgeon with the U.S. Central Command, thinks the military, which sells “truckloads” of body-building supplements at its bases, should not be selling them at all.
And how did the industry respond?
Part of the problem is lack of any pre-market requirement of proof of safety and part of the problem is retailers like GNC, who aren’t regulated at all. As reported in the Times, both had predictable responses to the lawsuit and unfavorable publicity, as did the supplement industry.
The attorney for USPlabs said the company is “unaware” of any deaths from the proper use of Jack3d and that there is no evidence the reported deaths were caused by the product. Various spokespersons for GNC, which had about $4.2 billion in revenue last year, said the company had no reason to believe that DMAA is unsafe, that GNC sells legal products widely available from other retailers, and that it complies with all relevant regulatory guidelines. A spokesperson for the Council for Responsible Nutrition, an industry trade group, said that a majority of supplements are safe.
Unfortunately, all of these speakers are well within their rights. Manufacturers are under no obligation to test their supplements to see if they are fatal before they market them and they must report any deaths only if someone happens to complain. Even then, they are free to say there is no proven causal relationship. And if the FDA wants to challenge that, the FDA has the burden of proof. No doubt GNC does comply with all regulatory guidelines as there aren’t any regulations requiring retailers to inquire into safety or effectiveness. The Council spokesperson is probably right when he says that a majority of supplements are safe. We just don’t know which ones aren’t until we find out the hard way, when injury and death reaches a threshold that spurs further investigation. Or, as Dr. Amy Eichner, a special adviser to the anti-doping association for American Olympic athletes, told the Times:
No consumer can ever know what’s inside a bottle. We advise our athletes that all supplement use is at their own risk.
Great advice for all consumers, whether athletes or not. In fact, what we need instead of the Quack Miranda Warning on supplement labels is a more accurate disclaimer of FDA involvement in dietary supplement regulation:
FDA WARNING: Safety and effectiveness unknown. Use at your own risk.
