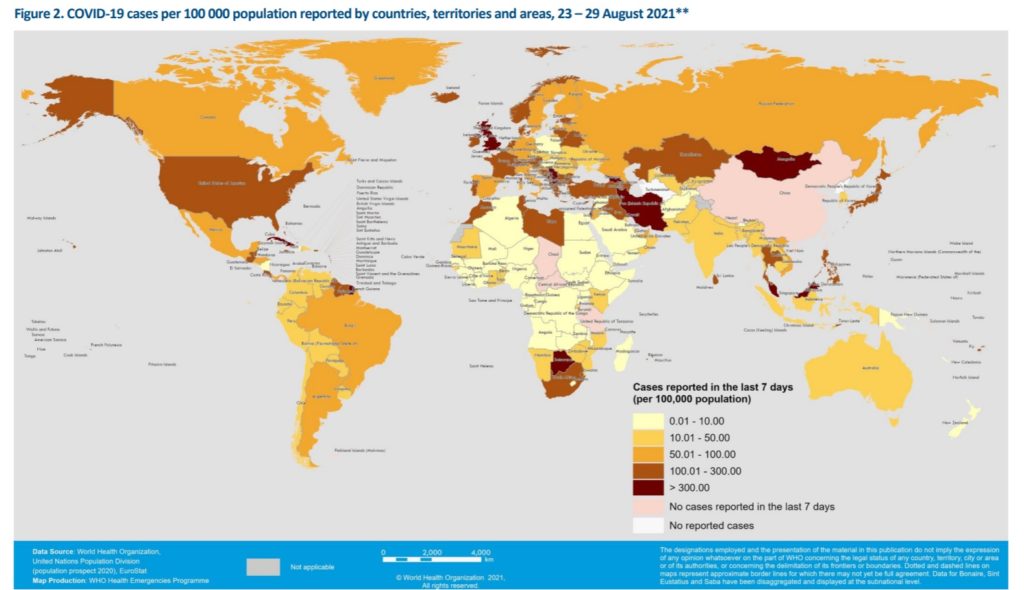
A snapshot of COVID cases as of August, 2021
No, this is not (unfortunately) about Loki and the Time Variance Authority (although I do recommend this series if you like that sort of thing). Rather, there are more COVID variants beyond Delta, and we need to keep an eye on them. It was just three months ago I wrote about the Delta variant, and we are now living through a new COVID Delta variant surge. But delta is not the final letter of the Greek alphabet, nor is the SARS-CoV-2 virus limited by such linguistic conventions.
Variants are simply versions of the virus with different properties due to mutations in one or more genes. These mutations may have a number of effects – making the virus more or less deadly, more or less easy to spread, more or less able to evade the host’s immune system, or the ability to survive in different environments, for example. Experts have warned throughout the pandemic that the longer it continues, the greater the probability of random mutations producing new variants that will perpetuate, and even worsen, the pandemic. The Delta variant has shown that warning to be absolutely true.
A recent study in Nature shows that the Delta variant is less sensitive to neutralizing antibodies produced from earlier variants. This kind of mutation is referred to as “immune escape” because it allows the virus to bypass (at least partially) host immunity. This is partly why the Delta variant is more infectious; more of the virus is allowed to replicate, so there is simply more virus in those droplets of water we spread around to each other. The virus is also better at replicating, and hangs out in those droplets longer. The result is that people infected with the Delta variant have about 1,000 times the virus in their system, and are about twice as likely to spread COVID as the original variant. Further, while the vaccines are still effective against the Delta variant, they are less so.
The World Health Organization (WHO) designates “variants of concern” if they demonstrate one or more of the following properties: increased infectivity or virulence, or evasion of one or more public health measures to limit spread (masks, distancing, vaccines). So far there are four variants of concern, alpha through delta. A “variant of interest” is used for:
[Variants] with genetic changes that are predicted or known to affect virus characteristics such as transmissibility, disease severity, immune escape, diagnostic or therapeutic escape; AND
Identified to cause significant community transmission or multiple COVID-19 clusters, in multiple countries with increasing relative prevalence alongside increasing number of cases over time, or other apparent epidemiological impacts to suggest an emerging risk to global public health.
They now list Eta, Iota, Kappa, Lambda and Mu as variants of interest. In short, variants of interest have mutations that might cause the virus to become more infectious or deadly, while variants of concern definitely do have such properties. One of the variants of interest, however, deserves special attention.
Mu variant
The Mu variant of SARS-CoV-2 was first detected in Colombia in January 2021. It has since spread to 40 countries, and currently represents only 0.1% of new infections. Colombia has the highest percentage, at about 39%. Currently in the US the Mu variant represents 0.2% of infections, with the Delta variant responsible for >99%. There is some good and bad news with the Mu variant, which is representative generally of what can happen with variants during a pandemic.
First the bad news – the Mu variant is a variant of interest because it has mutations to the spike protein that gives coronaviruses their ability to infect humans. As the WHO reports:
The Mu variant has a constellation of mutations that indicate potential properties of immune escape. Preliminary data presented to the Virus Evolution Working Group show a reduction in neutralization capacity of convalescent and vaccinee sera similar to that seen for the Beta variant, but this needs to be confirmed by further studies.
Some of these mutations are to locations where the vaccines are typically targeted. Not only, therefore, does this raise the possibility of immune escape but specifically of vaccine resistance escape. But as stated above, so far preliminary tests show this capacity is similar to the Beta variant.
The good news is that so far the Mu variant is not outcompeting the Delta variant. Even if the Mu variant has some very concerning properties, it might simply be outcompeted by the Delta variant, which is very contagious. This is what makes variants so hard to predict. No one mutation is going to give a virus an entire suite of properties, making them more infectious, virulent, and deadly all at the same time. A new variant may emerge that is very competitive in terms of infectivity, but mild in terms of severity. Or, a deadly virus may emerge that never gets a foothold against other more competitive variants.
But the more we allow variants to emerge because we fail to tamp down the pandemic adequately, the greater the probability of (by chance) a variant emerging that does have several bad properties all at once. Another concern is that different variants may target different subpopulations. The major concern for the Mu variant is that it may significantly evade COVID vaccines. If this is the case, then it may spread among the vaccinated, who are relatively protected from the otherwise more infectious Delta variant. There are too many possibilities to accurately predict what will happen. The WHO simply has to monitor and study variants as they emerge, and that’s what they are doing.
In the end the majority of experts predict that COVID will simply become endemic. We have already passed the point of being able to stop the pandemic, and it will now become like the flu or other circulating coronaviruses – here to stay. However, this does not mean it remains as it is today. Through infections and vaccines, the world’s population will become increasingly resistant to COVID. This will not be enough to stop it, and new variants means the virus will be constantly escaping immunity. But like the flu, it will probably settle down to a background infection we all have to live with, but will not mean lockdown and disruption.
It will likely change our lives. I expect, as a health care worker, wearing a mask to work is now the new normal. We will likely see masks out in public as a permanent fixture, and this is probably a good thing. If you have the sniffles or a fever, or have been exposed to someone who has COVID, stay home or if in doubt wear a mask. People will probably wear masks in large indoor or close crowds. And now we have a new vaccine to fight over, and hopefully most people will do the responsible thing and just get their annual booster (or whatever turns out to be optimal).
And now for something completely different – good news
To end on some good news – early reports from Israel suggest that getting a third dose or booster shot has a significant effect in reducing their current wave of COVID. Scientific research has provided the tool to fight this pandemic. Vaccines work. Get vaccinated.


