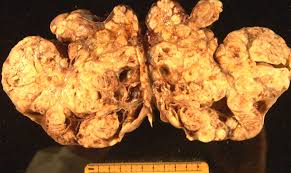
Ovarian cancer
Ovarian cancer is relatively rare but deadly. The lifetime risk of ovarian cancer is 1.5% compared to 12% for breast cancer, but it is the 5th most common cause of cancer death for women. Since the ovaries are hidden deep in the pelvis and the symptoms of ovarian cancer are non-specific, the cancer is often advanced by the time it is diagnosed and survival rates are low. Early detection by screening would be expected to improve outcomes. Two screening methods have been proposed: the cancer antigen CA-125 blood test, and pelvic ultrasound. The Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial (PLCO) found that screening with CA-125 and ultrasound did not reduce ovarian cancer mortality. The USPSTF recommends against screening for ovarian cancer because it does not reduce mortality and carries important potential harms from false positives and unnecessary surgeries.
Ovarian cancer screening is being re-considered in the light of a recent study, the UKCTOCS trial, published in The Lancet in December 2015. On the basis of that study, a test called ROCA is being offered directly to the public for $295. It’s important to understand what the study actually found, and why experts have questioned the wisdom of offering this test to the public at this time.
The UKCTOCS study
The letters stand for United Kingdom Collaborative Trial of Ovarian Cancer Screening. It was a randomized controlled trial with over 200,000 postmenopausal subjects. Half got no screening; a quarter got annual pelvic ultrasound; and a quarter got annual multimodal screening (MMS). In multimodal screening, changes in CA-125 levels were interpreted with an algorithm to assess ovarian cancer risk. Women found to be at high risk were further evaluated with repeat CA-125 tests and/or ultrasound. There was a trend to reduced mortality from ovarian cancer (15% in the MMS group and 11% in the ultrasound group), but the trend did not reach statistical significance. MMS was more sensitive than simply measuring CA-125 with a cut-off value, as had been done in previous studies; there were fewer unnecessary surgeries. The reduction in mortality appeared only after 7-10 years of screening. There was a stage shift: more cases were diagnosed at an early stage with MMS. The authors found their results encouraging, but they pointed out that:
Further follow-up is needed to assess the extent of the mortality reduction before firm conclusions can be reached on the long-term efficacy and cost-effectiveness of ovarian cancer screening.
The reaction of experts
In February 2016 a panel of experts convened at the Banbury Center, Cold Spring Harbor Laboratory, to discuss the implications of the study’s findings. They concluded that it was premature to recommend MMS at this time. They said:
Although women and health care professionals may look to these findings as finally providing a strategy for successful screening for ovarian cancer, the study investigators and participants at this meeting believe that screening policy requires a sound scientific foundation, which we currently do not have.
In June 2016, American Family Physician published an excellent review article on the diagnosis and management of ovarian cancer. They recommended that women at average risk should not be screened, and that women at high risk because of family history should be referred for genetic counseling. Additionally they recommended against routine screening pelvic examinations in asymptomatic women.
Accompanying that article were two editorials. One was signed by all the Banbury participants. They concluded:
The ROCA, a component of the MMS strategy evaluated in the UKCTOCS trial, is already commercially available. Although no organization recommends ovarian cancer screening in average-risk women, some women may wish to undergo periodic screening for ovarian cancer with CA 125 testing; therefore, health care professionals must advise women regarding the potential benefits and risks as we understand them now. Given the gaps in the evidence, the majority of Banbury participants were uncomfortable with direct-to-consumer advertising of an ovarian cancer screening test at this time.
The other editorial, by AFP editor Jay Siwek, was more forceful, saying that the ROCA protocol used in the study had been commercialized and promoted to the public in an unqualified way. He pointed out these shortcomings:
- The reduction in ovarian cancer mortality was not statistically significant.
- The reduction was not constant over time.
- Only one-fourth of the patients were followed long enough to begin to see a possible benefit.
- The effect of screening on all-cause mortality was not reported.
- The ROCA is a proprietary algorithm patented by the investigators.
And he concluded:
In keeping with the principles of the Choosing Wisely campaign, physicians and patients would do well to avoid the pitfalls of overscreening and wait for results that promise more hope than hype.
Conclusion
The ROCA protocol looks promising, but the evidence is preliminary. It’s not yet ready for prime time.

