A large number of vaccines are recommended for children; not so many for adults. Lately a new shingles vaccine has been added to the schedule for adults over the age of 50. The first shingles vaccine, Zostavax, was released in 2006. Now the FDA has approved another vaccine, Shingrix. You may be wondering if you really need to be vaccinated and if so, which vaccine to choose. Here are the facts, so you can make an informed decision.
Shingles and post-herpetic neuralgia
Shingles, or herpes zoster, is a late consequence of chickenpox. After chickenpox infection or vaccination with a live attenuated virus, the patient develops immunity, but an inactive form of the varicella virus (VZV) can persist in nerve cells in the sensory ganglia and can be reactivated later in life when the immunity to VZV wanes. The reactivated virus travels down the nerve and causes painful blisters in the dermatome, the section of skin served by that nerve. A serious long-term complication of shingles is post-herpetic neuralgia (which can sometimes even develop in the absence of a shingles rash!). It typically lasts 1-2 months but one-fifth of cases last a year or longer. It can be very painful and can have complications like aseptic meningitis. There is no cure; the pain is treated with painkillers, anticonvulsants, steroids, topical remedies, and antidepressants, often in combination.
Shingles is not transmitted from person to person, but exposure to a patient with shingles can cause chickenpox in someone who has never had chickenpox or the chickenpox vaccine.
What are my chances of getting shingles or post-herpetic neuralgia?
The incidence of shingles is 4 cases per 1,000 people per year; for those 60 and older, the incidence rises to 10 cases per 1,000 people per year. 1-4% of people with herpes zoster get hospitalized for complications. The fatality rate is 0.28 to 0.69 per million population, mostly in the elderly and the immunocompromised. It can recur: 1-5% of patients will go on to have a second or even a third episode.
Herpes zoster rates are increasing, and some have tried to blame routine vaccination of children, suggesting that adult immunity is more likely to wane when adults are not occasionally exposed to children with chickenpox. But the CDC has determined that rates started increasing before varicella vaccine was introduced, and they did not accelerate after routine varicella vaccination was started. And other countries that don’t routinely vaccinate against chicken pox have observed similar increases in herpes zoster rates.
According to the Clinical Evidence Handbook in American Family Physician:
The main risk factor for postherpetic neuralgia is increasing age. The condition is uncommon in persons younger than 50 years. However, among persons who have had acute herpes zoster, it develops in 20 percent of those 60 to 65 years of age and in greater than 30 percent of those older than 80 years.
Up to 2 percent of persons with acute herpes zoster may continue to have postherpetic pain for five years or more.
Oral antiviral agents (acyclovir, famciclovir, valacyclovir, and netivudine), taken during acute herpes zoster infection, may reduce the duration of postherpetic neuralgia compared with placebo.
Zostavax vs. Shingrix
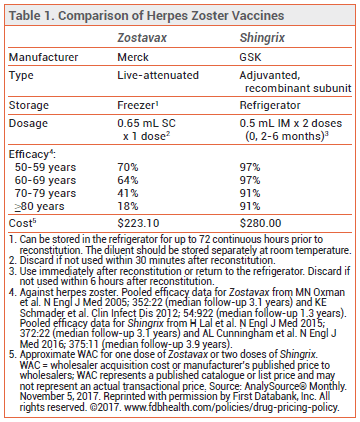
The first zoster vaccine to be licensed, Zostavax, contains live attenuated VZV that cannot cause the full-blown disease but can create immunity. Rarely, it can cause a rash or a mild case of shingles. Live vaccines are contraindicated in immunocompromised patients because they can cause complications. The new vaccine, Shingrix, does not contain live virus, so it is not contraindicated for immunocompromised patients. It is a recombinant vaccine containing a surface VZV antigen obtained from genetically engineered Chinese hamster ovary cells, an antigen that triggers a targeted immune response to VZV. It also contains an adjuvant that enhances the immune response. It is more effective than Zostavax but requires two doses instead of one. The Medical Letter published this handy chart comparing the two vaccines and showing the efficacy for different age groups:
Adverse effects
Systemic adverse reactions to Zostavax were only slightly greater than with placebo. Shingrix appears to cause more adverse effects: 17% had severe local reactions that prevented normal daily activities for an average of 2 days. Other reported effects included myalgia (45%), fatigue (45%), headache (38%), shivering (27%), fever (21%), GI symptoms (17%), injection-site pain (78%), redness (38%), and swelling (26%).
Recommendations
The CDC recommends Shingrix for all immunocompetent adults age 50 or older, even if they have previously had shingles or Zostavax.
Conclusion: More effective but more adverse effects
The new vaccine is more effective but causes more adverse effects. Some will welcome the additional “insurance” against a painful and relatively common condition. Others will be put off by the reported adverse effects. I am one of those. I have never refused a vaccine before, but I looked at the odds for my personal situation. I have had shingles, so there is at least a 95% chance that I won’t get it again. I have had the Zostavax vaccine, so I’m protected to some extent. I don’t plan to get Shingrix;I’ll wait for them to develop another vaccine that is equally effective with fewer side effects.
Shingrix is different from most vaccines in that it only protects the person who is vaccinated. Most other vaccines protect others in the community through herd immunity, and I strongly recommend them because of their public health consequences. I have personally decided not to get the new shingles vaccine, but that shouldn’t influence the decisions of others. I am neither recommending nor “not” recommending it. I encourage everyone to do what I did: look at the facts and make a personal decision based on their own situation and preferences.

