[Editor’s note: The COVID-19 crisis brings us a double-dose of Dr. Weinberg this week, with a timely post about hydroxychloroquine.]
In recent weeks an obscure drug has become the subject of much attention and debate in the public arena. The drug is called hydroxychloroquine. Hydroxychloroquine and a closely relative drug, chloroquine, are members of a class of chemicals known as quinolines. These drugs were long-ago recognized as anti-malarials. Chloroquine, in particular, was used extensively during WWI for the treatment and prophylaxis of malaria.

Chloroquine (from pubchem.ncbi.nlm.nih.gov)

Hydroxychloroquine (from pubchem.ncbi.nlm.nih.gov)
Later, these drugs were recognized to be effective against certain autoimmune diseases, particularly rheumatoid arthritis and systemic lupus erythematosus. Patients with these chronic diseases are often on these medications for many years, much longer than typically required for malaria. With prolonged exposure a new adverse effect was recognized: a potentially blinding retinal toxicity. The first cases of retinal damage attributed to chloroquine was reported in 1957. Due to a superior safety profile, hydroxychloroquine has largely replaced chloroquine for treatment of autoimmune disease, but can produce retinal injury identical to chloroquine.
Retinal injury from hydroxychloroquine
Early detection is desirable because continued treatment can result in significant disability. The damage is often progressive long after the medication is stopped, probably because chloroquine and hydroxychloroquine have a strong affinity for pigmented tissues and remain sequestered for years after the medication is discontinued. The classic pattern of retinal toxicity is often referred to as bull’s-eye retinopathy (or bull’s-eye maculopathy) because the retina displays a concentric zone of decreased pigment surrounding the center of the retina (the macula, see image below). With conscientious monitoring, toxicity from hydroxychloroquine is usually recognizable before the patient becomes symptomatic.
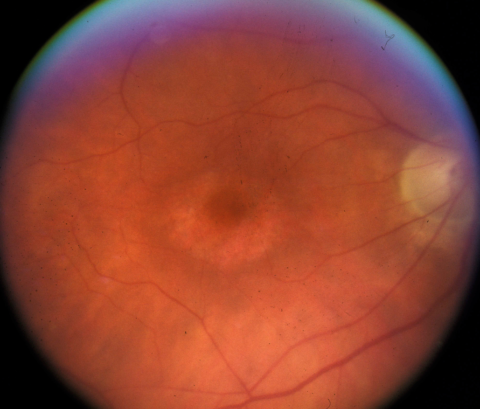
Photo of the retina of the right eye of a patient with hydroxychloroquine retinopathy. The paler concentric ring (near the center of the photo) is characteristic, and the reason hydroxychloroquine toxicity is frequently classified as “bull’s-eye” retinopathy. Loss of visual function accompanies the anatomic change.
An expert panel from the American Academy of Ophthalmology has issued recommendations for the hydroxychloroquine treatment and monitoring. The upper limit of the recommended dose was recently decreased to 5 mg/kg/day. If dosing guidelines are followed, the risk of toxicity is estimated to be <1% in the first 5 years, <2% up to 10 years. After 10 years the risk rises more steeply, up to 20% after 20 years. Higher doses confer a higher risk of toxicity. Baseline eye examination is recommended within 1 year of initiating therapy and annual screening exams beginning after 5 years of treatment. There are a couple of case reports of what appears to be hydroxychloroquine toxicity after only a couple of months of exposure, but these are very rare events.
Hydroxychloroquine and COVID-19
Due to the COVID-19 pandemic, “hydroxychloroquine” has become a household word. Based on some intriguing laboratory data and very preliminary clinical reports, hydroxychloroquine has emerged as a potential treatment for the novel coronavirus, prompting some high level government officials and other high profile personalities to advocate for widespread use. David Gorski has written several detailed analyses of the state of evidence (or lack thereof) for the efficacy of hydroxychloroquine for COVID-19, and I have nothing to add to his excellent review of the evidence. I agree that based on very thin data there is irrational exuberance among some prominent opinion-makers.
At this moment, there is no shortage of clinical trials looking at hydroxychloroquine in the context of COVID-19. A search on clinicaltrials.gov had 117 hits (as of 4/21/2020). The studies are from all around the world and have variable designs. Investigators are exploring intervention with hydroxychloroquine at various stages of infection, and some are looking at prophylaxis for known exposures and high-risk individuals. Many doses and schedules of treatment are being explored. I did not do a detailed review of all 117 studies, but I reviewed a sample. Most of the studies are looking at doses in excess of the American Academy of Ophthalmology recommended upper limit of 5 mg/kg/day sometimes by several multiples. Duration of treatment ranges from a few days to a few weeks.
Even at these high doses I suspect the risk of retinal toxicity with short-term exposure is low. There are, however, caveats to this conclusion. Patients with COVID may be critically ill and are likely to be on multiple medications. The potential retinal toxicity of hydroxychloroquine in critically ill, metabolically compromised, multiply-medicated patients is unknown. Considering the devastation seen due to COVID-19, the risk seems justified in the context of clinical trials. We can be hopeful that data from clinical trials will be responsibly collected, collated, and reported. I look forward to these data to inform us about the safety and efficacy of hydroxychloroquine for COVID-19.
Outside clinical trials, hydroxychloroquine is also being used, largely based on encouragement of a few high profile opinion-makers. I fear that some people, desperate to protect themselves, may take the medication at doses and durations sufficient to put them at risk for retinal damage (or even worse, die after drinking the wrong substance based on a misunderstanding). Meanwhile, patients with disabling diseases like rheumatoid arthritis and lupus are sometimes having difficulty filling their prescriptions.
Conclusion: Low short-term risk, but completely uncertain efficacy
The world desperately needs effective treatments for COVID-19. We can only hope that effective strategies will be discovered. This can only happen by using a science-based, systematic approach. Unless good data supporting the safety and efficacy of hydroxychloroquine emerge, there are many reasons to be cautious adopting it for widespread use. Fortunately, current knowledge suggests that the risk retinal toxicity from short-term exposure to hydroxychloroquine is low.

