Asthma can be serious, and needs to be managed with medicine, not magical thinking.
For the past few years I’ve been adding to what I call the naturopathy versus science series of posts, where I’ve been examining the public advice and writing by naturopaths on a particular topic, and contrasting it against the scientific evidence. I’ve focused on naturopaths instead of other “alternative-to-medicine” providers because naturopaths actively promote themselves as health professions capable of delivering primary care, akin to medical doctors. And in many parts of Canada and the United States they have been successful with this marketing, despite the fact that the naturopathic curriculum is filled with pseudoscience, and there is no convincing evidence to show that naturopathy offers anything that is uniquely useful or incrementally better than “conventional” medicine.
What I’ve learned from writing these posts has been sobering. I’ve looked at the naturopathic perspectives on fake diseases, infertility, prenatal vitamins, vaccinations, allergies, and even scientific facts themselves. While they can offer reasonable, science-based advice, naturopaths may also offer health advice that can be at odds with medical evidence and sometimes even basic laws of physics. Naturopaths claim to treat serious chronic diseases like diabetes, and their advice can range from sensible to the useless or potentially harmful.
Timothy Caulfield is a Canadian researcher who has done this type of work in a more systematic, structured way. A letter published a few years ago in Allergy, Asthma, & Clinical Immunology was one approach to understand the alignment between naturopathy and scientific standards. Caulfield and Christen Rachul found that the most widely-advertised practices in Alberta and British Columbia lacked a sound evidence base:
A review of the therapies advertised on the websites of clinics offering naturopathic treatments does not support the proposition that naturopathic medicine is a science and evidence-based practice.
Caulfield has a new paper that builds on his past study. He’s expanded the scan to include chiropractors, acupuncturists, and homeopaths, and has focused exclusively on treatment claims related to allergies, “sensitivities” and asthma. And what’s he’s identified raises concerns about the potential for ineffective and possibly harmful treatments being offered to consumers by these providers.
Fake medicine for real diseases can be deadly
Allergies and asthma can be mild conditions, but they can also be fatal. Asthma kills hundreds of thousands per year worldwide. It isn’t a disease that should be treated trivially, with treatments that don’t work. Yet that’s exactly what can happen when you don’t consider the scientific evidence supporting the treatments you use (or sell). Untreated (or under-treated) asthma can cause long-term lung damage. Fortunately there are demonstrably effective medications that can reduce the short- and long-term effects of asthma.
The best study I’ve seen that demonstrates how fake medicine can be perceived to treat real conditions was a study of placebo versus albuterol (an asthma medicine) and “fake” acupuncture versus “real” acupuncture in asthma patients. Rather than digress to this study (rather than the one I want to get to) I’ll point you to Peter Lipson’s post that summarizes it nicely. The bottom line from the study was that, not surprisingly, placebo can make an asthma patient feel better but when it came to objective measurements of actual effects on lung function, acupuncture (real or fake) offered no benefit whatsoever. This is an important finding and sets the context for Caulfield’s latest paper: Patients may report that they feel better when they use ineffective treatments like acupuncture, but these are placebo effects. To get real effects in the treatment of a condition like asthma, you must use real medicine. There are no objectively meaningful “placebo” effects.
Who are the providers?
For some of you that may not be regular readers of this blog, understanding the differences between alternative medicine providers may be helpful in interpreting this new paper, and the authors’ conclusions. Unlike what are called “allied health professionals” (e.g., nurses, pharmacists, physiotherapists, dieticians, speech language pathologists, etc.), alternative medicine providers offer services that do not share scientific and biomedical underpinnings with the conventional scientific medical model. The four mentioned in Caulfield’s new paper are:
Homeopaths: Homeopathy was invented by German physician Samuel Hahnemann in 1796. It is based on the belief that if you dilute something that causes your symptoms when healthy, it can cure those same symptoms when you are sick. The more you dilute the substance, the more powerful it is believed to become. Substances can range from coffee to vacuum cleaner dust or dolphin sonar. (Homeopaths, please let me know how you collect and bottle dolphin sonar.) Homeopaths believe the most powerful substances are those that are so dilute there is mathematically zero chance that any of the original substance remains. Homeopaths claim these remedies are effective because water is thought to retain a “memory” of the original substance. Not surprisingly, there is no convincing evidence that homeopathy is anything other than an elaborate placebo system.
Acupuncturists: Acupuncture is (most commonly) the practice of placing very thin needles in the skin in specific regions of the body. With Chinese origins, acupuncture is only several decades old as is currently practiced. While it is believed that pushing needles into designated areas is more effective than pretending to stick needles into people, the scientific evidence shows that “fake” acupuncture is just as effective as “real” acupuncture. There’s a lack of good evidence to show that acupuncture offers any meaningful medical effects beyond placebo effects.
Chiropractors: Chiropractic was invented by D.D. Palmer in 1895 and is based on the idea that the spine is connected to all other organs, so by manipulating the spine through the elimination of “subluxations” (which are identifiable only to chiropractors) that health can be restored to the body. Unlike acupuncture and homeopathy there is some evidence to suggest that the manipulation techniques used by chiropractors can be effective for some types of low back pain. However many chiropractors believe the can treat conditions for which there is no credible evidence that spinal manipulation can be effective.
Naturopaths: Naturopathy is an alternative medicine practice based on a belief in vitalism, the concept that living beings have a “life force” not found in inanimate objects. Naturopathic treatment ideas are all grounded in the idea of restoring this “energy”, rather than being based on objective science. Naturopathy has evolved to include practices like homeopathy and acupuncture, and also herbalism and Traditional Chinese Medicine. Pretty much anything goes in naturopathy (it’s not clear there is a naturopathic standard of care), as long as it is felt to align with the underlying naturopathic philosophy.
Selling falsehoods?
With this background in mind let’s now turn to a new paper by Blake Murdock, Stuart Carr and Timothy Caulfield at the University of Alberta. (I highly recommend Caulfields’s book A Cure for Everything?) Caulfield is one of the most outspoken Canadian critics of pseudoscience, particularly when pseudoscience masquerades as real medicine. This new paper is a straightforward cross-sectional analysis of marketing claims made by Canadian chiropractors, naturopaths, homeopaths and acupuncturists, entitled “Selling falsehoods? A cross-sectional study of Canadian naturopathy, homeopathy, chiropractic and acupuncture clinic website claims relating to allergy and asthma.” The paper was published in BMJ Open in December, 2016, and is open access.
The paper’s introduction describes the current context for complementary and alternative medicine (CAM) in Canada. Like other countries around the world, CAM highly popular, with chiropractic being by far the most popular practice accessed by Canadians (40% access in a lifetime, versus 17% for acupuncturists, 9% for naturopaths and 9% for homeopaths.) The authors note that while CAM providers are increasingly being described as primary care providers, that the scope of conditions that are claimed to be amenable to alternative medicine is both broad and largely unsubstantiated.
The researchers selected 10 large Canadian metropolitan areas and using the web tool isearchfrom.com, performed regional searches to identify CAM practitioner websites. Within the 400 websites, they analyzed them for the terms “sensitivity”, “allergy”, and “asthma,” and then looked for claims about the ability to treat these conditions. Here are the main findings, broken down by mention/claim and type of CAM provider:
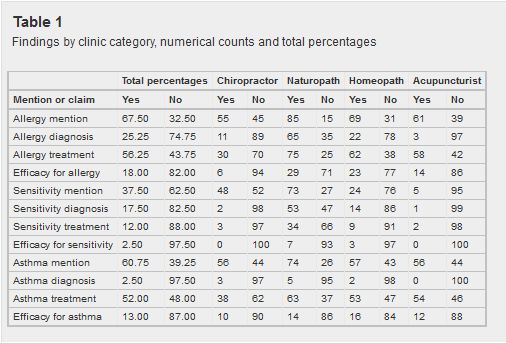
Table 1: Findings by type of provider
The majority of practitioners mentioned these conditions on their website, with the majority also claiming to treat allergies and asthma. Remarkably, about 75% of naturopaths claim to treat allergies and asthma despite the lack of unique “naturopathic” treatments that have been demonstrated to effectively treat these conditions. Also concerning are the substantial numbers of chiropractors, homeopaths, and acupuncturists who claim to treat allergies and asthma, despite the fact there are similarly no treatments that these practitioners offer which have been shown to offer any meaningful, objective benefits for these conditions. Despite this, efficacy claims are common:
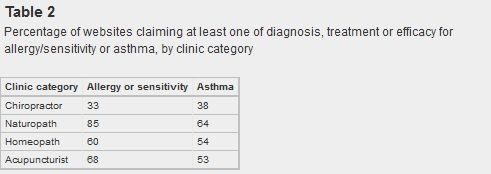
Table 2: Percentage of websites claiming at least one of diagnosis, treatment or efficacy
The authors go on to break down the results by geographic region, which I’ll defer comment on other than to observe that Vancouver seems to be CAM central when it comes to claims about efficacy and treatment. More interesting (and concerning) is the list of tests and treatments recommended for the treatment of allergies, sensitivities and asthma. While disclaimers were noted on some websites, explicit claims were also made about the ability of these practitioners to diagnose and treat these conditions:
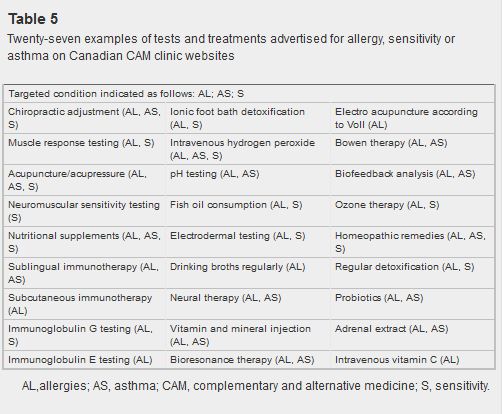
Table 5: Twenty-seven examples of tests and treatments advertised by chiropractors, acupuncturists, naturopaths and homeopaths for allergy, sensitivity or asthma
Not surprisingly, there’s a lack of evidence to support many of these treatments, which the authors note raises ethical questions. Live blood analysis, Vega testing, intravenous vitamins, and homeopathy are all clinically useless for the diagnosis or treatment of these conditions. The authors correctly point out that not only can this lead to dietary changes that may be harmful (particularly in children), that these types of treatments may result in greater healthcare demands overall and even the financial exploitation of consumers who may be led to believe these tests and treatments are of value.
Use caution when evaluating claims
Despite the growing acceptance of CAM and CAM providers, there is persistent evidence that the interventions advertised by chiropractors, acupuncturists, naturopaths and homeopaths lack evidence of effectiveness. To date, in Canada and worldwide, there have been few attempts to hold these providers accountable for the claims that they make, and the tests and diagnoses that they offer. The authors suggest a number of strategies that could be considered, including more effective regulation of advertising, as well as considering specific approaches to protect minors. Ultimately until there is the recognition that these providers and practices may be harmful, this remains an area where consumers must be very cautious. Given the findings of this paper, it would seem prudent to discuss the use of CAM providers or treatments for allergies, sensitivities or asthma, with health professionals, preferably ones that are legitimate specialists in these conditions.
Images via flickr users Carolina Biological Supply and KristyFaith used under a CC licence.
