![]() I don’t recall if I’ve mentioned it on SBM before, but I went to the University of Michigan. In fact, I didn’t go there just for undergraduate studies or medical school, but rather for both, graduating with a B.S. in Chemistry with Honors in 1984 and from medical school in 1988. In my eight years in Ann Arbor, I came to love the place, and I still have an affinity for it, even though it’s been over 20 years since I last walked about the campus as a student, although I have been back from time to time for various functions, most recently to see Brian Deer speak last winter. True, I’m not fanatical about it, as some of my contemporaries and friends who attened U. of M. with me back in the 1980s (and, sadly, the string of losses to Ohio State and the definitively mediocre last season Michigan had last year make it very hard to be a Michigan football fan these days). However, I do have considerable affection for the place. It molded me, trained me in science, taught me medicine, and provided me the basis for everything I do professionally today.
I don’t recall if I’ve mentioned it on SBM before, but I went to the University of Michigan. In fact, I didn’t go there just for undergraduate studies or medical school, but rather for both, graduating with a B.S. in Chemistry with Honors in 1984 and from medical school in 1988. In my eight years in Ann Arbor, I came to love the place, and I still have an affinity for it, even though it’s been over 20 years since I last walked about the campus as a student, although I have been back from time to time for various functions, most recently to see Brian Deer speak last winter. True, I’m not fanatical about it, as some of my contemporaries and friends who attened U. of M. with me back in the 1980s (and, sadly, the string of losses to Ohio State and the definitively mediocre last season Michigan had last year make it very hard to be a Michigan football fan these days). However, I do have considerable affection for the place. It molded me, trained me in science, taught me medicine, and provided me the basis for everything I do professionally today.
I mention all of this because I’ve become very disappointed with the University of Michigan Medical School of late. The reason is that it’s “distinguished itself” as a leading institution teaching and promoting the mish-mash of sometimes mutually contradictory modalities, the vast majority of which are either based on mysticism or pseudoscience, known commonly as either “complementary and alternative medicine” (CAM) or “integrative medicine” (IM). The University of Michigan Integrative Medicine Program (UMIM) describes itself thusly:
University of Michigan Integrative Medicine, an interdisciplinary program, is committed to the thoughtful and compassionate integration of complementary therapies and conventional medicine through the activities of research, education, clinical services and community partnerships. As a healing-oriented approach to medical care, integrative medicine takes into account the whole person (body, mind, spirit and emotion), including all aspects of lifestyle.
The vision, mission and values of the University of Michigan Integrative Medicine (UMIM) program reflect our belief that patients and our community are best served when all available therapies are considered in concert with an approach that recognizes the intrinsic wholeness of each individual. It also reflects our belief that the best medicine is practiced in collaboration with a wide variety of healthcare professionals and with our patients.
Alas, my alma mater could well be featured in Kim’s old feature, the Weekly Waluation of the Weasel Words of Woo (W5). Indeed, look at the medical student curriculum supported by this program:
Supported by a five-year grant from the National Institutes of Health (NIH), University of Michigan Integrative Medicine (UMIM) piloted its first Complementary and Alternative Medicine (CAM) courses for medical students during the Fall Term of 2000. A unique aspect of the CAM course sequence is that it is longitudinal, extending across the entire four-year U-M Medical School curriculum.
To date, implementation of the curriculum has involved the participation of approximately 600 undergraduate medical students and 200 physicians/practitioners. Instruction has touched upon the following five CAM domains as identified by the National Center for Complementary and Alternative Medicine (NCCAM):
- Alternative medical systems
- Mind-body interventions
- Biologically based therapies
- Manipulative and body-based methods
- Energy therapies
Energy therapies? As you can see my alma mater, my beloved U. of M., appears to have wholeheartedly embraced what Dr. Robert Donnell has referred to as “quackademic medicine.” Indeed, it now has a fellowship in IM that is described thusly:
Fellows design elective experiences in integrative medicine using resources found within the university health care system. Topics may include (but are not limited to): Aromatherapy, Health System Management, Herbal Therapies, Holistic Nutrition, Integrative Pharmacy, Manipulative Therapies, Mind-Body Medicine, and Naturopathic Medicine. Fellows also participate in weekly formal learning activities through U-M Integrative Medicine and the Department of Family Medicine.
Financial support is provided to achieve competency in one defined core curricular area.
[…]
Graduates of this program will model best practices in integrative health care by embracing healing-oriented medicine that takes into account the whole person (body, mind and spirit), including all aspects of lifestyle. This philosophy emphasizes therapeutic relationships and recognizes use of all appropriate therapies, both conventional and alternative.
W5 indeed. Notice how no mention is made of science or the scientific basis of any of these therapies. To read the educational objectives is to see just how little science matters in IM.
All of this is yet another in the series of my characteristically self-indulgently logorrheic introductions to an analysis of a study. It turns out that U. of M. is trying to do something resembling science about CAM. The problem is that, like many investigators and universities do, it’s falling for the same problems and fallacies when true believers try to do what Harriet Hall has so delightfully termed “Tooth Fairy science.” I never thought I’d be saying it, but it looks as though my alma mater is doing a bit of the ol’ Tooth Fairy science. Several readers sent me this study, and, since it came from U. of M., I figured it falls upon me, among the SBM bloggers, to take it on. Let us start with how I found out about this study, a credulous article published last week and entitled Acupuncture boosts effects of painkillers, natural or prescription:
High-tech images of the brains of chronic pain sufferers have found that the ancient practice of acupuncture fights pain by making key brain cells more sensitive to the pain-dampening effects of opioid chemicals. The study, published online in the August issue of the journal NeuroImage, comes less than a year after the publication of a controversial study that concluded acupuncture was no more effective than sham treatment at reducing pain.
Researchers at the University of Michigan’s Chronic Pain and Fatigue Research Center used a positron emission tomography (PET) scanner to view the brains of 20 women diagnosed with fibromyalgia who reported suffering nerve and muscle pain at least 50% of the time. The PET scans were conducted during each woman’s first acupuncture session and, a month later, her eighth.
In the regions of the brain that process and dampen pain signals — the amygdala, caudate, cingula, thalamus and insula — the PET scans showed an increase in the receptivity — and possibly the number — of brain cells to which opioid substances bind. Study author Richard E. Harris said that suggests that acupuncture appears to make the body more responsive to opioid painkillers.
It turns out that Dr. Harris is not only a molecular biologist but a licensed acupuncturist, which goes to show just how much people can compartmentalize science and belief, walling them off from each other. There are, not unexpectedly, methodological problems with this article that render its conclusions questionable, but in reality it’s more a problem of interpretation. There’s a famous line from The Princess Bride, where the character Inigo Montoya says of a word, “I do not think it means what you think it means.” In the case of this study, I would paraphrase that famous line to say, “I do not think your results mean what you think they mean.” Here’s why.
Harris acknowledges up front that several studies have now shown acupuncture to be no more efficacious than sham acupuncture. Indeed, we have written about such studies right here on SBM that show that acupuncture is no more effective than sham acupuncture. It doesn’t matter if the sham acupuncture is needles inserted in the “wrong” acupuncture points or fake needles that do not penetrate the skin or even toothpicks. The most reasonable scientific conclusion from all of these studies is that acupuncture, as practiced by adherents of traditional Chinese medicine, does not work. At the very best, it’s a nonspecific effect that doesn’t rely on anything resembling a system. More likely, acupuncture is nothing more than an elaborate placebo. None of this, however, stops Harris’ group from trying to show that there is a different between sham acupuncture and real acupuncture at some sort of level, and this study is their attempt to do just that. Here is the background as Harris states it in the introduction to his study, entitled Traditional Chinese acupuncture and placebo (sham) acupuncture are differentiated by their effects on μ-opioid receptors (MORs):
Recent controversy in the field of acupuncture research was generated when several large scale randomized controlled trials in chronic pain patients failed to show superiority of acupuncture over sham acupuncture methods (Brinkhaus et al., 2006; Linde et al., 2005; Melchart et al., 2005; Harris et al., 2005). This has lead opponents of acupuncture therapy to suggest that it is no more effective than a placebo intervention. Since placebo administration also induces activation of opioid receptors, specifically the μ-opioid receptor (MOR) class (Benedetti and Amanzio, 1997; Zubieta et al., 2005; Amanzio and Benedetti, 1999; Levine et al., 1978; Pomeranz and Chiu, 1976), acupuncture may indeed operate in part via placebo mechanisms.
There’s almost certainly no “may” about it, and you can also almost certainly safely scratch “in part,” but that’s just me being a nasty skeptic or, as I like to think, a good scientist. I also find it curious why Harris would refer to investigators who are telling it like it is, so to speak, and pointing out accurately what these studies show “opponents” of acupuncture. It suggests a bit of an adversarial, defensive, “I’ll show you” mindset right from the start.
Be that as it may, the hypothesis to be studied is that long term acupuncture therapy somehow results in increased μ-opioid receptor availability and that this effect would not be seen in a sham acupuncture group. Harris chose fibromyalgia (FM) patients for his study because previous work of his had shown that FM patients have reduced central μ-opioid receptor (MOR) binding potential. In that study patients with greater clinical pain were found to have reduced MOR binding potential, and Dr. Harris wondered if acupuncture could somehow increase that binding potential and thus relieve pain. Thus, this study is the classic example of a researcher taking a technique developed for the study of one question and applying it to another question, and what Harris asks is whether acupuncture and sham acupuncture have different (or any) effects on these receptors. Specifically, the technique used is positron emission tomography (PET) designed to look at the binding of opioids to these receptors using 11C-carfentanil (CFN) positron emission tomography (PET) with the μ-opioid selective radiotracer [11C]carfentanil.
The study involved randomizing 20 women with FM into one of two groups, either sham acupuncture or “real” acupuncture. Subjects were blinded to which group they were in, but investigators were not, and a questionnaire was given to see if patients could guess what group they were in. The results in each group were no more accurate than random chance, suggesting that patient blinding, at least, was good. It was not clear to me, however, from the text whether those who were evaluating the PET scans were also blinded to which experimental group each patient was in. That is such a mind-numbingly obviously necessary part of designing any imaging experiment such as this that I will assume that the physicians reading the scans were in fact blinded to what experimental group each scan came from, but it’s disturbing that this very basic experimental design point wasn’t explicitly stated anywhere. Also, it’s clear that the investigators doing the acupuncture or sham acupuncture were not blinded. There are now retractable sham needles available that do a pretty good job of hiding from even acupuncturists whether a real needle went in or not; I wonder why those weren’t used.
In any case, there were no significant differences between the groups with respect to demographics or initial pain scores, and patients were excluded who: had previous experience with acupuncture; had current use or a history of use of opioid or narcotic analgesics; had a history of substance abuse; had the presence of a known coagulation abnormality, thrombocytopenia, or bleeding diathesis that may preclude the safe use of acupuncture; had the presence of concurrent autoimmune or inflammatory disease; had concurrent participation in other therapeutic trials; were pregnant and nursing mothers; had severe psychiatric illnesses; or had contraindications to PET. Outcome measures included clinical pain scores using the Short Form of the McGill Pain Questionnaire and measures of μ-opioid binding.
As in many other studies of acupuncture versus sham acupuncture, non-insertional sham needles were used for the sham acupuncture procedure. Patients underwent a total of nine acupuncture or sham acupuncture treatments over the course of a month, undergoing PET scans at treatment #1 and tretament #9. At each of the two PET sessions, study participants first underwent a baseline scan for minutes 10-40 after infusion of the radiotracer, then the acupuncture or sham procedure, then another scan at 45-90 minutes. The researchers reported both short term increases in μ-opioid binding in various parts of the brain involved in sensory processing, including the cingulate, amygdala, insula, thalamus, and caudate. Longer term increases in MOR binding were also observed in a subset of the same structures, including the cingulate, caudate, and amygdala. There were no such increases in the sham acupuncture group, and in some regions small reductions of MOR binding were observed. Consistent with the other acupuncture studies that Harris mentioned, there was no difference in pain scores between the sham and “true” acupuncture groups.
Well, at least that much is consistent with previous results.
Here’s one big problem with this study. Needles were retained for the acupuncture group, but there were no needles in the sham acupuncture group because no needles had been inserted. It’s not clear to me from the methods whether the sham needles were left attached to the skin or not. Even if the subject were blindfolded, as these subjects were, I would think that would be very important in order to make the groups as much “alike” as possible. Whatever the true case was, the fact remains that, during the second PET scan period there was a definite difference between the two groups. The “true acupuncture” group had needles sticking into their skin at acupuncture points. The sham acupuncture group did not. Couldn’t that more or less completely explain the short term results? In essence, what Harris studied was differences in neurobiology between subjects who had needles sticking out of their skin and those who did not.
Here’s the second big problem. Take a look at this figure, which is Figure 1B from the paper:
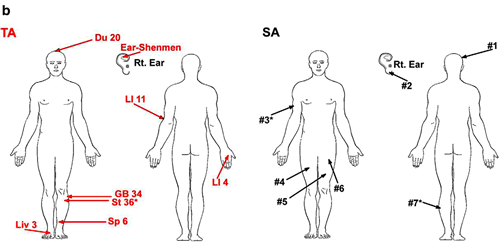
Notice something? The “true acupuncture” (left side, in red) procedure is not only different from the sham in that the sham doesn’t actually insert any needles. It uses different locations! The text calls them “similar” because they are in the same body part. Not how, for example, sham point #1 is on the head, but not in the same location as Du 20); sham point #2 is on the ear but on the earlobe instead of the pinna; sham point #3 is on the anterior surface of the right arm instead of the posterior surface of the left arm; most of the sham points in the leg are on the thigh, rather than the lower leg, where the “true” acupuncture points are.
Does anyone see a problem with this?
I do. In designing a good placebo control for an acupuncture study (or any other randomized clinical study), you shouldn’t, if you can possibly help it, mix and match changes in the procedure to produce your sham procedure. When you choose a sham acupuncture procedure, either insert the needles as usual in the “wrong” places or use the sham needles that don’t pierce the skin in the “right” places. Or have two groups and compare both. Don’t place sham needles that don’t pierce the skin in the “wrong” places. That’s two differences between the sham procedure and acupuncture and opens the door to a lot of confounders. Again, couldn’t this using a sham procedure that uses the “wrong” points and needles that don’t pierce the skin also partially explain the results of this study? Couldn’t the combination of using different locations and no insertion for the sham confound the results sufficiently as to render the results of this study virtually meaningless. I argue that they potentially can. I can’t prove it, but certainly the methodological shortcomings of this trial make it hard to take as any definitive evidence that there is different neurobiology going on between real acupuncture and sham acupuncture. All it does is to show that maybe there is a neurobiological difference between having needles sticking out of the skin and not having needles sticking out of the skin, which would be of little surprise, although the exact difference could be of interest. What this study does not show is that acupuncture “works.” I suppose it’s possible that sticking needles in the skin may have nonspecific effects that might alleviate pain, but this very study shows that they are no different than placebo. After all, there was no difference in pain relief between subjects receiving sham acupuncture and real acupuncture. Both experienced the same amount of subjective pain relief!
Not that that stops Harris from trying to imply that sham and true acupuncture “work” through different mechanisms:
Another intriguing result from the present study is that although MOR BP values were differentially altered by TA and SA, reduction in clinical pain was similar between groups. In a clinical trial, when an active treatment does not exhibit superior efficacy to a sham or placebo, the active treatment is assumed to be ineffective and only operating via a placebo effect. However this study suggests that this may be an erroneous conclusion. In this instance, our non-insertion sham procedure evoked a similar reduction in pain as our true acupuncture and we speculate that this occurred via a different mechanism. The analgesic effects of SA could have been due to regional reductions in MOR BP, consistent with activation of this class of receptors during placebo effects (Zubieta et al., 2005), whereas TA evoked an increase in receptor binding availability.
Alternatively, the perceived pain relief accorded by sham acupuncture and true acupuncture could be occurring by placebo mechanisms entirely unrelated to the observation of this study, which may have had nothing to do with the clinical placebo effects seen. That’s a rather more simple explanation for these results than all that handwaving (and, yes, it is mostly handwaving) in the paragraph above. I’m rather surprised the reviewers didn’t make Harris revise his manuscript to consider this possibility and discuss it. Harris could be correct. I doubt that he is, but he could be. However, my alternate explanation could also be correct. Moreover, even if he is correct, so what? It might be intellectually interesting and useful for understanding the placebo effect to determine the differences in neurobiology underlying two different placebo treatments, but none of this validates acupuncture as anything more than an elaborate placebo. It’s also a long run for a short slide, so to speak, in that nine sessions in a month of sticking needles into the body seems a lot to undergo for such minimal results based on such tenuous mechanisms.
It’s also depressing to see how the press has spun this study. Reports on the study are more or less reporting it exactly as Harris represented his results in the Discussion section of his paper. I have yet to see a news story with anything more than a very token skeptical view. Instead, they all proclaim this study as evidence that acupuncture can somehow crank up the level of opioid receptors to the point where they make opioid drugs work better. Heck, the article I cited said that this study shows that acupuncture can increase the efficacy of opioid analgesics, either natural or prescription! There’s zero evidence presented in this paper that shows that.
This paper represents to me the latest in a line of rationalizations of acupuncture. Acupuncturists start out saying that “acupuncture works” based on nonblinded studies for which placebo effects are not adequately controlled for. Then, when better studies show that true acupuncture is no better than sham acupuncture (or, amusingly, sometimes that the sham acupuncture “works” better), they rationalize it by saying either that the sham was not a good sham or that these studies don’t say anything because sham acupuncture “works” too. Harris takes a different tack in saying that, yes, there’s no difference in perceived pain due to sham acupuncture or true acupuncture not only because they both work but because they both work by different physiological mechanisms. He might have had a (weak) point were it not for his seemingly willful misinterpretation of his results and his changing too many things at the same time in his sham control group. Instead, all he’s shown is that opioid receptors light up more if there are needles in the skin than they do if there are not–hardly a finding that shows that acupuncture “works” and certainly not any sort of finding to validate the entire system of acupuncture, which relies upon the idea of qi flowing through meridians, flows that can be altered to therapeutic effect by sticking needles into those meridians.
“I do not think your results mean what you think they mean,” indeed.
REFERENCE:
Harris, R., Zubieta, J., Scott, D., Napadow, V., Gracely, R., & Clauw, D. (2009). Traditional Chinese acupuncture and placebo (sham) acupuncture are differentiated by their effects on μ-opioid receptors (MORs) NeuroImage, 47 (3), 1077-1085 DOI: 10.1016/j.neuroimage.2009.05.083
ADDENDUM: Christina Stephens at the JREF Swift Blog has written a good analysis of this study.
