Insomnia can be a persistent issue for both children and adults. While there are a few over-the-counter and multiple prescription drugs used for insomnia, many people are understandably apprehensive about using them. Tell someone there’s “natural supplement” for sleep, and there’s usually a lot of interest. That’s what I’ve seen with melatonin, a hormone that is sold without a prescription in many countries. It is widely perceived as safe and effective and many health professionals recommend it for treating sleeping problems in both adults and children. In the United States, sales of melatonin have increase from $285 million in 2016 to $821 million in 2020. With this growing popularity the number of pediatric poisonings reported to poison control centres has also increased. In 2020, melatonin also became the most frequently-reported pediatric poisoning reported. A new report from the Centers for Disease Control and Prevention documents how these poisonings are causing an increase in serious adverse effects.
In the early 1900s it was observed that the pineal gland secreted a substance with physiologic effects, and the hormone itself was named in 1958. Receptors for the hormone have been identified in the hypothalamus, the pituitary, and in other organs in the body. And it’s definitely a natural substance: melatonin is found in vertebrates, invertebrates, animals, bacteria, fungi, algae and plants. In humans and other mammals, melatonin secretion by the pineal gland follows the light cycle, being low during daylight hours, surging in the evening and peaking in the middle of the night. This secretion starts in infancy and continues through adulthood, followed by a decline as we age. It has been explored in clinical trials mainly for the prevention and treatment of sleep disorders like insomnia and jet lag. The evidence suggests melatonin is modestly effective. It seems to be most effective for sleep-onset insomnia, and may give a slight increase in total sleep time. In children melatonin may be recommended for long-term use in autism spectrum disorder and attention deficit hyperactivity disorder.
Melatonin is generally very well tolerated. The most common side effects reported include daytime sleepiness, dizziness and headaches. Melatonin’s long-term effectiveness and safety are not clear. Given melatonin is a hormone, and receptors for this hormone are distributed throughout the body (including the sex organs), the safety, particularly during puberty, has not been established. So the advice is to use with caution and when necessary. Moreover, given the problems with quality of dietary supplements in many countries, there are legitimate concerns about product consistency and safety.
Poison control center reports
This new paper, published by the CDC in Morbidity and Mortality Weekly Report, is a study of all pediatric and young adult (<19 years old) melatonin ingestions reported to poison control centers in the United States between 2012 and 2021. During that period, 260,435 ingestions were reported, representing 2.25% of all reports. Ingestions were primarily in those <5 years old (84%), were unintentional 94% of the time, and occurred in the home 99% of the time. Reassuringly, most ingestions were without any symptoms (84.4%). When side effects were reported, the most common effects were central nervous system, gastrointestinal, and cardiovascular.
Of the 260,435 ingestions, 27,795 were treated at a health care facility. 71.6% were discharged, 14.7% were hospitalized, and 1% (287 cases) required intensive care unit support. Five children required mechanical ventilation, and two children died. Both of those children were under the age of two.
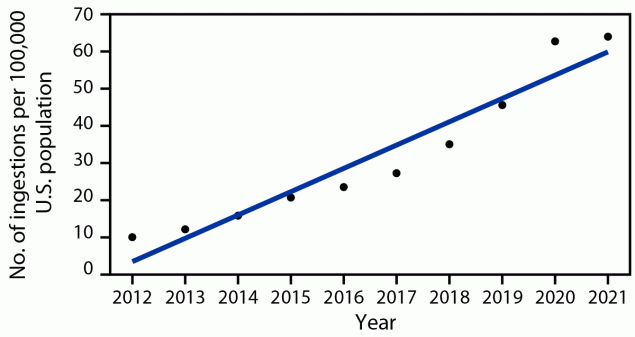
Interestingly, the largest increase in ingestions occurred between 2019 and 2020. (The authors speculate that this could conceivably have been driven in part by stay-at-home orders, school closures, and pandemic-related sleep disturbances.) By 2021, melatonin was accountable for almost 5% of all poisonings reported to poison control centers, compared with 0.6% in 2012. It’s a linear trend:
FIGURE 1. Rate* of pediatric† melatonin ingestions reported to poison control centers, by year§ — United States, 2012–2021
* Ingestions per 100,000 population, based on U.S. Census Bureau Annual Estimate.
† Aged ≤19 years.
§ Linear trend, p<0.001.
The authors noted the following limitations with their analysis: (1) data is collected based on self-reports that may underestimate actual exposures (2) poison control centers are not able to verify the accuracy of all case reports, and (3) poison control data does not allow one to confirm if deaths are due to the toxic effects of melatonin or because of other factors.
In the discussion, the authors discuss the quality control issues that have been identified with supplements, including melatonin, where products may not match the labelled claim. Given melatonin is treated as a dietary supplement in the United States, it continues to be marketed without manufacturing being held to “drug-like” standards for quality, consistency, and even packaging.
Treat melatonin like a drug
Melatonin is considered innocuous, safe, and effective, and its use has exploded over the last decade. There is widespread use and marketing of melatonin for children and it is even available in “gummy” form for that population. Likely due to growing popularity and use, accidental ingestions are increasing in frequency. While these products may not be packaged in child-resistant containers or considered to be potentially harmful, health professionals and consumers alike should be aware of the risks of melatonin toxicity and take steps to avoid accidental poisonings.