Determining the net health effects of independent factors can be tricky, especially when those factors cannot be controlled for in experimental studies. For things like body mass index (BMI) we must rely on observational data and triangulate with multiple studies to isolate the contributions from BMI. But it can be done.
The data, however, are likely to be complex and noisy, and therefore there is plenty of opportunity for ideology to trump objectivity in interpreting the data. There are those who, for whatever reason, deny that we are having an obesity epidemic in the West, and those who deny the health implications of being overweight as an independent factor.
BMI
The terms overweight and obesity have had various definitions in the past, but in recent years the various health organizations have settled on consensus operational definitions (for obvious practical reasons). Their definition relates to body mass index, which is a person’s weight in kilograms (kg) divided by their height in meters (m) squared.
It should be noted that BMI is a measure of weight, not fat (adiposity). BMI is used for convenience, as height and weight data are often available, but more direct measures of body fat are not. It is widely recognized and admitted that BMI is problematic as applied to individuals. Muscular and athletic people may have a high BMI and not have excess adiposity, for example. Also at the extremes of height the BMI becomes harder to interpret.
But this does not mean the BMI is useless. In fact, for most people BMI correlates quite well with adiposity. In one study researchers compared BMI to a more direct measure of body fat percentage using skin-fold thickness. They found that when subjects met the criterion for obesity based upon BMI, they were truly obese by skin-fold thickness 50-80% of the time (depending on gender and ethnicity). When they were not obese by BMI they were not obese by skin-fold 85-99% of the time.
So BMI is a rough but useful estimate, good for large epidemiological studies where more elaborate fat percentage measurements are not practical. However, those who wish to deny the “obesity epidemic” have found BMI to be a convenient target for sowing doubt.
There is ongoing research into the utility of supplementing BMI with other easy measures, like waist circumference. This seems to be a more accurate measure of adiposity, and specifically risk from being overweight. So going forward we may see more meaningful measured routinely captured, and BMI may be replaced or supplemented with these measures. But for now we will continue to see many studies based upon BMI.
Overweight and Obese
Because BMI is a convenient measure, it has become the measure of choice in defining overweight and obesity. For children and adolescents overweight is defined as a BMI in the 85-95% percentile by age and gender, while obesity is >95% percentile BMI. For adults overweight is defined as a BMI of >=25.0 but <30.0, obese is defined by BMI >=30.0 and < 40.0, and extremely obese is defined as BMI >=40.0.
These cutoffs, like all such cutoffs for medical definitions, are partly arbitrary (they constitute drawing a line to demarcate a spectrum) but are evidence- based. This is similar to definitions for hypertension, for example. Researchers typically will set the cutoff to capture most people who are at risk for medical complications.
This is where the controversy comes into play with overweight and obesity. In 1998 the NIH decided to lower the cutoff for BMI for overweight, from 28 for men and 27 for women to 25 for both sexes. This was based upon an expert panel review of hundreds of studies. It also brought the NIH definition in line with the World Health Organization and other health organizations. The BMI 25 cutoff has now become generally accepted. The cutoff for obesity was not changed – it was and remains a BMI of 30.
Of course this means that any estimates of overweight (but not obesity) based upon the newer lower cutoff of BMI 25 would be greater than estimates based upon the previous criteria. This raised a bit of a kurfuffle, as it always seems to do when medical definitions are altered. This happened with the lowering of the cholesterol cutoff, blood pressure for hypertension, and blood sugar for diabetes.
This event in 1998 now has become a central argument in the arsenal of obesity deniers. If you search on “obesity statistics”, on the first page you will get this apparent libertarian site which quotes a “food industry spokesman” as saying:
In 1998, the U.S. Government changed the standards by which body mass index is measured. As a result, close to 30 million Americans were shifted from a government-approved weight to the overweight and obese category, without gaining an ounce, Burrita said.
This is slightly misleading, as the obese category was not changed. But the main point is that this 1998 redefinition is being used to argue that the obesity epidemic is all smoke and mirrors. The article goes on to quote this gem from William Quick:
According to an American Medical Association report, 14.5 % of Americans in 1980 were obese, a total of 32,700,000 (based on a population of 226,000,000). If, as the above article states, the numbers of obese Americans have “doubled” in the past twenty years, this would mean there are now about 66 million of them. But thirty million of those fatties were created by a change in definition, so by the standards of 1980 [we would calculate an] obesity percentage of 12.85 percent, an actual decrease in obesity percentage since 1980.
That’s some massively flawed reasoning. Again we see the confusion of the overweight and obese categories. But also there are many false assumptions in that back-of-the-envelope calculation. Quick is mixing statistics from different sources and contexts, and the result is a mess.
What we really need is a look at the numbers over time using the same definition. Fortunately, most epidemiologists are not dolts and they get this very basic concept. In fact, it doesn’t get much more basic than this, and it would take some pretty naive incompetence to use inconsistent definitions over time.
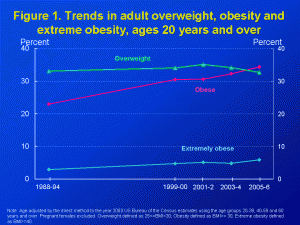 The CDC has crunched the numbers for us, and using the modern cutoffs for overweight, obese, and extremely obese applied to BMI data for the last few decades they document a pretty steady increase in American fatness over time. Take a look at the video on the site to see this data presented graphically. Also, it is summarized in the graph here.
The CDC has crunched the numbers for us, and using the modern cutoffs for overweight, obese, and extremely obese applied to BMI data for the last few decades they document a pretty steady increase in American fatness over time. Take a look at the video on the site to see this data presented graphically. Also, it is summarized in the graph here.
As you can see, the lines go steadily up – with the exception that the overweight category has decreased in the last decade. However, it seems that this is due to the shifting of people from the overweight category to the obese category, not to the normal weight category.
Of course, you could cherry pick by just looking at the overweight category. Looking at all the data, however, tells the real story.
The Health Risks of Overweight
Is being overweight and obese an independent risk factor for any specific illness? The answer is an overwhelming yes. There are many diseases for which being overweight is a risk factor, such as type II diabetes, obstructive sleep apnea, pseudotumor cerebri, heart disease, and other illnesses. The data is clear – but complex, and so allows for those motivated to deny the connection to distort and cherry pick the data to create the impression they wish.
From a website advocating size acceptance we read:
There is actually no evidence that being fat will give you diabetes or cancer or PCOS or any other health issues. Being obese tends to correlate with some health problems, but the causes of the health problems may be multiple, and they certainly aren’t thoroughly understood in current medical research.
It must be pointed out that many obese people are perfectly healthy, if you look at the numbers that matter. This seems to refute the idea that fat alone causes artery clogging, diabetes, or anything else it’s often blamed for – clearly, there are at least other factors besides fat, and it may even be the case that fat’s nothing to do with it at all. As long as your other numbers are good, your weight does not impact your health. If you can possibly afford to get your numbers tested once a year, or even every few years, do so. If the numbers that matter are good, your weight is fine
Here we see a couple of logical fallacies. The first is the denial of cause based upon an overapplication of the “correlation does not equal causation” fallacy. It is true that correlation alone does not prove causation, but causation may be the answer, and we can test this hypothesis by testing multiple correlations. For example, if weight is reduced will the risk of the disease decrease.
Also, the fact that being overweight and obese may cause health problems through intermediary effects is irrelevant. If being overweight causes insulin resistance which causes diabetes, it is not meaningful to say that weight is not causing diabetes.
We also see confusion between weight as a risk factor vs being an absolute cause. Weight is one factor among many, such as genetics. There are obese people who are otherwise healthy, just like there are heavy smokers who never get lung cancer. This is entirely irrelevant to the claim that weight is a risk factor for various diseases. The lack of 100% correlation does not justify the conclusion that weight has “nothing to do with it at all.”
Conclusion
There is an obesity epidemic in the US and in developed nations generally, and this increase in adiposity is an independent risk factor for many diseases and disorders. Exactly what role weight is playing in specific diseases is a complex question that is the subject of ongoing research, but there is already overwhelming data in many condition to show that being overweight is a health risk.
Further – this has nothing to do with size acceptance. We can separate the question of social stigma from the medical facts. It is also folly to tie a social/ethical issue to a specific factual premise – because when the facts don’t come out the way you wish that either weakens your ethical stance, and/or forces you to deny the scientific facts. We can simultaneously treat overweight and obesity as the health problem that it is, while addressing the social and psychological aspects of weight in our society.


