And now for something completely different.
Any time the skin is violated, there is the possibility of infection. Surgeons, of course, have known this ever since they started taking sharp objects to skin, either to remove limbs or organs or rearrange anatomy for therapeutic intent. We also know that the risk of a surgical site infection (SSI) varies depending on the procedure. Today that knowledge is codified into surgical wound classifications:
- Clean: These surgical wounds are uninfected and without preexisting inflammation, and tracts where bacteria might reside (e.g., respiratory, GI, GU tracts) are not entered. These wounds are closed primarily; i.e., stapled or sewn closed at the end of the procedure. Examples: Removal of skin lesions, mastectomy, thyroid surgery, hernia repair, splenectomy.
- Clean-contaminated: These are wounds in operations in which the respiratory, GI, or GU tract is entered, but in a planned, controlled fashion. There is no unusual contamination with the contents of those tracts, because they are entered in a controlled fashion and contamination is minimized. Examples: Cholecystectomy, small bowel resection, Whipple operation, gastric surgery, lung surgery, colon surgery.
- Contaminated: These wounds occur in cases such as dealing with open, fresh accidental wounds; cases in which there is a major break in sterile technique, gross spillage from the GI tract or acute nonpurulent (no pus) inflammation.
- Dirty: “Dirty cases” are, as you might imagine, quite dirty. They include, for example, old traumatic wounds with devitalized tissue; existing bowel perforation, infection, or even gross abscess. The point is that the gross contamination and organisms are present before the procedure begins. Examples: Incision and drainage of an abscess, repair of perforated bowel, peritonitis, wound debridement, and the like.
The higher the surgical class, in general, the higher the risk of a postoperative wound infection. Or so surgical dogma has traditionally taught (more on that later). Also, in general, preoperative antibiotics are administered before cases that are class 2 (clean-contaminated) or above, and primary closure of the skin is generally not recommended for class 3 (contaminated) and above. As is true of so many things in medicine, the rules are not necessarily hard and fast, but this is the simple version taught to medical students. Also, determining what does and doesn’t work in terms of preventing SSIs has turned out to be not as easy as one would think. There’s a lot of dogma here, and recommendations have changed over the years.
SSIs, not surprisingly, have become a focus of quality improvement, with great effort, particularly by the American College of Surgeons’ National Surgical Quality Improvement Program (ACS NSQIP®). I’d like to focus on just one controversy that’s been brewing over the last few years that (finally, I hope) has probably been resolved and in doing so have what I hope to be a fun change of pace from my usual rants. So today I will be discussing a fairly focused topic and a major study that was just published in the August issue of the Journal of the American College of Surgeons addressing a critical question: Bouffant vs Skull Cap and Impact on Surgical Site Infection: Does Operating Room Headwear Really Matter? In other words, does the choice of headgear to keep that nasty hair of yours away from the surgical field matter? (Spoilers: It doesn’t.) Before we get to the study, let’s take a look at the debate and its history.
Skullcap versus bouffant?
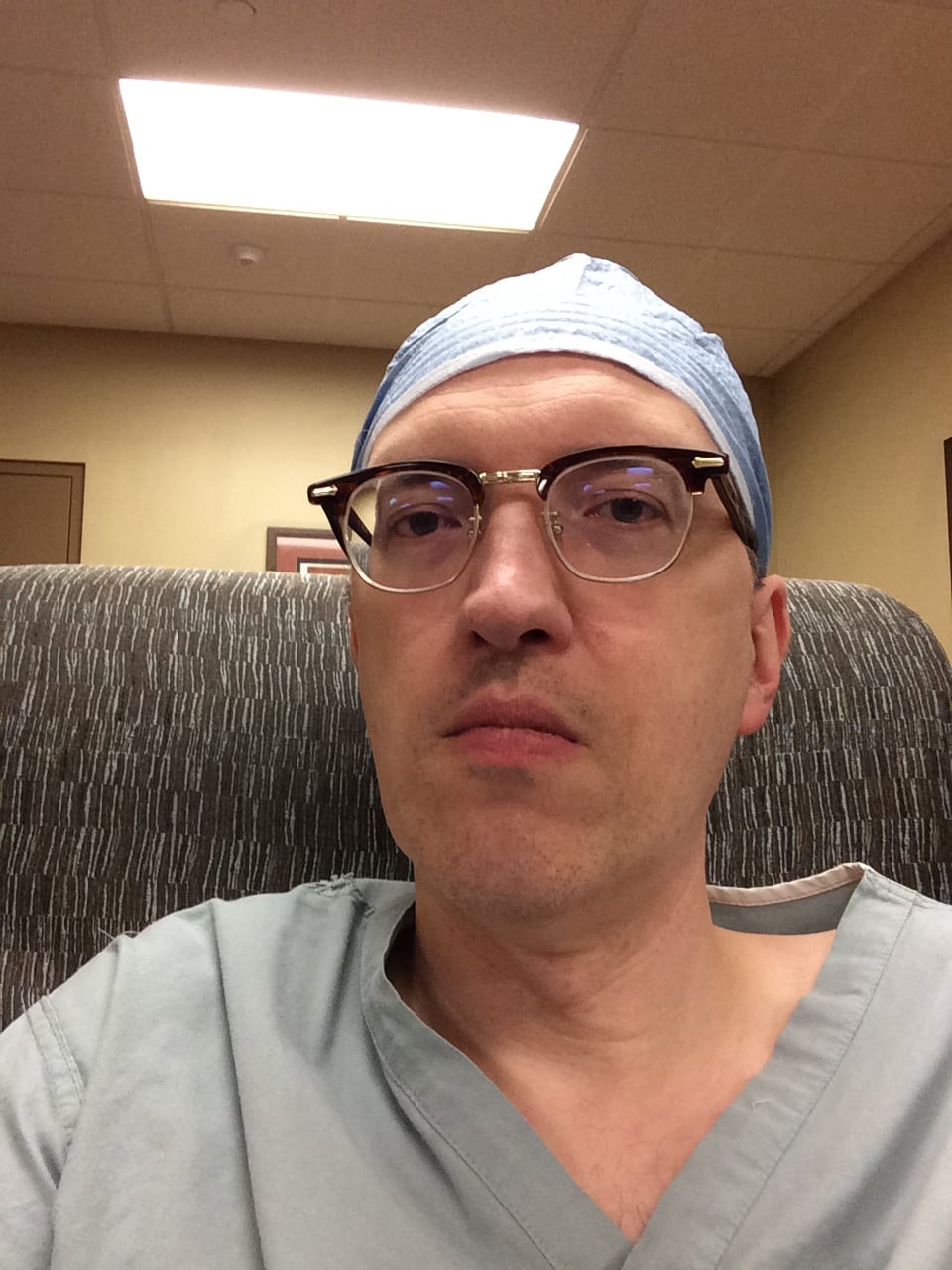
Anyone who’s been in the operating room (or watched medical dramas on television) is probably aware that surgical headgear comes in two forms: the skullcap or the bouffant. The skullcap generally looks like this:
As you can see, it’s tight and lean and actually fairly good-looking. Indeed, here’s a selfie I took a few years ago, before my hospital got rid of the surgical skullcap (and before I grew my current beard):
Not bad, if I do say so myself. I almost look like a real surgeon in this photo.
Then there’s the bouffant cap. You can actually see one in the picture above, but the head of the woman who’s wearing it is partially obscured by the surgeon wearing the skullcap. Here’s another surgeon wearing a bouffant cap:
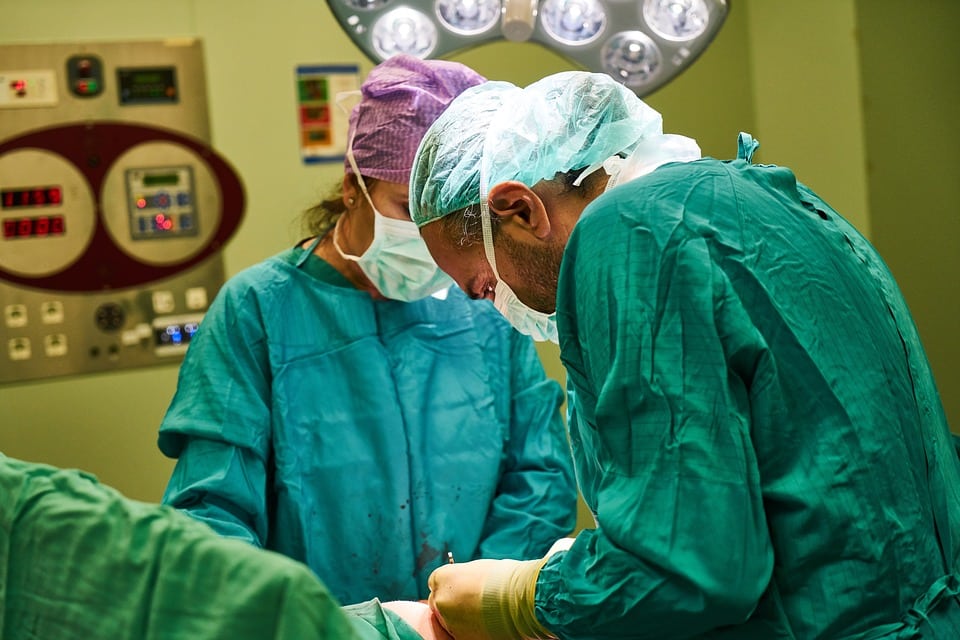
If you don’t choose a bouffant cap, you’re going to be giving your patients nasty infections, or so AORN seems to be saying.
As you can see, it’s basically a much looser-fitting cap with elastic to keep it on the head. Most older surgeons, particularly male surgeons, also detest it.
Throughout my nearly 30 years as a surgeon (if you count my residency), I’ve used both varieties of caps. I tend to prefer the skullcap because it’s better-fitting for someone with short hair, and the bouffant cap tends to migrate on my head as I move around doing operations. The one downside to the skullcap is that it flattens my hair to the point that, when I come home after a day in the operating room, my wife sometimes makes fun of my “operation head”.
Why, you might ask, should anyone care about this? If you don’t work in an operating room, there’s probably no good reason to care. Among those of us who do, the issue has become, rather oddly, a pretty passionate debate. For example, take a look at this article from two years ago in the Boston Globe:
Surgeons for years have stepped into operating rooms wearing their surgical cap — a snug covering that ties in back and comes in standard-issue blue or hundreds of personalized designs.
But a crackdown appears to be underway on that almost sacred piece of headgear.
Inspectors in January reprimanded operating room staff at Brigham and Women’s Hospital in Boston for having the hair around their ears uncovered during surgery — and for sporting visible facial hair. And a New York surgeon was written up for showing 3 inches of hair at the nape of his neck.
For sure, other operating room staff wear surgical caps, but they have long been the hat of choice for many surgeons. The problem is the hats usually leave small amounts of hair and the ears exposed — a situation that an influential nursing group says could promote infection.
Regulators have taken the nurses’ concerns to heart, forcing some hospitals to switch to shower cap-like “bouffants,’’ which can be pulled down over a wearer’s entire head.
To be honest, I’ve never really used a cloth skull cap in the operating room, and whenever I’ve seen a surgeon sporting one I always wondered when the last time it had been washed was. If such a cap, no matter how spiffy the design, hasn’t been washed after every one or two days of use, personally I couldn’t help but think: Ew. So instead, I wore the disposable paper caps.
Basically, what we’re looking at here is an ongoing spat between the Association of periOperative Registered Nurses (AORN) and surgeons, represented by the American College of Surgeons. AORN guidelines in practice ban the skull cap and require the bouffant cap, while ACS guidelines state that skull caps with minimal hair exposure are acceptable. Why do I say the AORN guidelines ban the skull cap “in practice”? Continue reading and find out.
Cage match: ACS vs. AORN
To be honest, I’ve rarely seen a tiff between two professional organizations over a surgical guideline based on so little evidence and infused with much emotion. Reading each side’s position statements while writing this post, I had a hard time not concluding, “A pox on both your houses”. (I realize that some surgeons will likely view me as a traitor or apostate for saying that. Such is life.) In any case, let’s look at the ACS response to AORN’s guidelines. First, it is remarkable how much broad agreement there was between the two organizations. On the other hand, I was a bit embarrassed at how the ACS stated that its “guidelines for appropriate attire are based on professionalism, common sense, decorum, and the available evidence”. Why is evidence listed last? And who cares about common sense? However, here are the areas of general agreement, except for some quibbling around the edges, which I won’t discuss in detail:
- Soiled scrubs and/or hats should be changed as soon as feasible and certainly prior to speaking with family members after a surgical procedure.
- Scrubs and hats worn during dirty or contaminated cases should be changed prior to subsequent cases even if not visibly soiled.
- Masks should not be worn dangling at any time.
- Operating room (OR) scrubs should not be worn in the hospital facility outside of the OR area without a clean lab coat or appropriate cover up over them.
- OR scrubs should not be worn at any time outside of the hospital perimeter.
- OR scrubs should be changed at least daily.
- During invasive procedures, the mouth, nose, and hair (skull and face) should be covered to avoid potential wound contamination. Large sideburns and ponytails should be covered or contained. There is no evidence that leaving ears, a limited amount of hair on the nape of the neck or a modest sideburn uncovered contributes to wound infections.
- Earrings and jewelry worn on the head or neck where they might fall into or contaminate the sterile field should all be removed or appropriately covered during procedures
- The ACS encourages clean appropriate professional attire (not scrubs) to be worn during all patient encounters outside of the OR.
Now here’s another kicker. The ACS response stated:
The skullcap is symbolic of the surgical profession. The skullcap can be worn when close to the totality of hair is covered by it and only a limited amount of hair on the nape of the neck or a modest sideburn remains uncovered. Like OR scrubs, cloth skull caps should be cleaned and changed daily. Paper skull caps should be disposed of daily and following every dirty or contaminated case. Religious beliefs regarding headwear should be respected without compromising patient safety.
Indeed, among surgeons, much is made in this debate about how the skull cap is presumably the “symbol” of the surgical profession, and maybe it is—or was, at least when back when nearly all surgeons were men with short hair. These days, an increasing percentage of surgeons are women, most of whom presumably have longer hair and can’t use a skull cap because it doesn’t cover their hair adequately. To argue in 2016 that the skull cap is the “symbol” of the surgical profession revealed a blindness to the reality of surgery today. Maybe the skull cap was once the “symbol” of the surgical profession, but I would argue that, even if that was once the case, it shouldn’t be any longer. Stick to the evidence and not some emotional attachment to the days of yore, when men were men and women, by and large, were not surgeons. Also, most of the people in the operating room are not surgeons. There are nurses, scrub techs, anesthesiologists, nurse-anesthetists, and the like. They probably don’t care if the skull cap is a “symbol” of the surgical profession. Yes, we surgeons tend to think we’re the center of the universe.
Indeed, all too often the surgeons’ argument basically boiled down to “I like it and have been doing it this way for 20 years,” even if the surgeon has to stretch quite a bit to make reasons that boil down to, “I don’t like bouffant caps” sound like something else:
None of that is to say that the AORN position, at least with respect to surgical caps, is particularly evidence-based. (Unfortunately, you have to be a member of AORN to see the actual statement on the AORN website. WTF, AORN?) Take a look at its response to the ACS guidelines, particularly the part where it responds to the statement about how the skull cap is symbolic of the surgical profession:
Wearing a particular head covering based on its symbolism is not evidence-based, and should not be a basis for a nationwide practice recommendation. Several types of evidence exist that support recommendations that perioperative personnel cover their head and ears in the OR. This evidence includes the fact that human skin and hair is naturally colonized with many bacteria, and perioperative personnel shed microorganisms into the air around them. We know airborne bacteria in the OR can fall into the operative field, contribute to the overall air contamination of the OR, and place patients at risk of surgical site infections. Completely covering the hair can reduce the number of bacteria introduced into OR air by perioperative personnel.
I’d say that the ACS needs an icepack for that burn, compounded by AORN’s other retort that, “until an evidence-based definition of ‘limited’ or ‘modest’ can be determine[d], there is no way for facilities to enforce such a recommendation” that only “limited” hair can be left uncovered.
However, despite invoking “evidence-based” definitions, notice that AORN didn’t cite any actual…oh, you know…evidence to show that wearing surgical skull caps is associated with an increased SSI rate. It makes a not unreasonable argument in terms of how the skin and hair are colonized with bacteria and how surgical personnel can shed them. However, that’s an argument that pretty much relies on prior probability. Yes, it’s not unreasonable to point out that exposed hair might shed bacteria onto the surgical field. However, surgeons used to do a lot of things to decrease SSI rates based on ideas that seemed to make sense at the time but were later found in controlled studies either to make no difference or to be counterproductive. Extensive shaving of the surgical site, particularly the night before, comes to mind. Nowadays, we don’t shave surgical sites unless there’s a lot of hair, and then we only just use clippers to cut it very short right before surgery, right before the surgical prep with antiseptic solution.
There was at the time of AORN’s recommendations basically no evidence suggesting that choice of surgical headgear influences SSI rates. Even the Boston Globe story noted that two large reviews of published studies in the last five years before 2016 showed little or no evidence that surgeon surgical headgear choice affected SSI rates. It also noted AORN’s argument that there can’t be any randomized controlled trials because such a trial “would potentially expose patients to the risk of infection from health care workers whose skin and hair were uncovered…” I agree that such a study would be impractical, but not for that reason. There is what I would call genuine clinical equipoise in the question; we honestly didn’t know if headgear made a difference in SSI rates and the evidence to that point suggested that it probably did not. AORN was way off-base in claiming that such a trial would be unethical because of lack of clinical equipoise. The real reason it would be impractical is because no one would want to agree to be randomized to one type of cap or another. Logistically, such a study would be a nightmare.
Let’s come back to the problem. In practice, the AORN guidelines for surgical attire have resulted in the banning of the use of surgical skull caps. Why do I say “in practice”? The reason is simple. AORN’s recommendations have been, in essence, adopted by the Joint Commission on Accreditation of Healthcare Organizations (JCAHO), the organization that accredits hospitals in the US, and the Agency for Healthcare Research and Quality (AHRQ), the U.S. Department of Health and Human Services agency dedicated to research and evidence-based guidelines to improve the safety and quality of health care. Remember that story above? Who were the inspectors who cited the hospitals for violations of surgical headgear standards? JCAHO. As a result:
After it became aware of the increased scrutiny, Beth Israel Deaconess Medical Center in Boston took away surgeons’ traditional scrub hats. Dr. Daniel Jones now wears a bouffant pulled down over his ears — but he’s not thrilled about it. “Doubt the ear hairs pose any threat,’’ he said in an e-mail. “Some actually wear a scrub hat under the bouffant to dress it up.’’
And that’s what’s happening all over the country. The OR leadership in my own hospital declared that skull caps would no longer be allowed, again, based on no evidence.
Amusingly, AORN is a bit annoyed at this whole controversy. Indeed, last year, it issued a statement denying that its guidelines ban the use of skull caps. It pointed out that the 2014 guidelines stated, “A clean surgical head cover or hood that confines all hair and completely covers the ears, scalp skin, sideburns, and nape of the neck should be worn.” AORN bases this recommendation on the observation that hair can harbor bacteria that can potentially fall into the surgical field. Indeed, AORN took great umbrage at the suggestion that it has “banned skull caps” in its statement, lamenting how its position had been “misrepresented” in media reports. If this PowerPoint presentation on the official AORN template on getting rid of the skull cap and advocating for bouffant caps instead is any indication, AORN was most definitely advocating for getting rid of the skull cap.
The study
At this point, readers who aren’t regulars and don’t appreciate my tendency towards liking to pontificate on the history of an issue before getting to the study under consideration are probably annoyed that I haven’t gotten to the point yet. So here we go, let’s get to it: “Bouffant vs Skull Cap and Impact on Surgical Site Infection: Does Operating Room Headwear Really Matter?”
The authors note in the introduction the factors associated with increased risk of SSI:
Approximately 300,000 surgical site infections (SSIs) occur each year, accounting for approximately one-third of hospital-acquired infections.1, 2, 3 Many factors contribute to this, including surgery type, glucose control, and patient body temperature. Recent attention has been given to the type of headwear as a risk factor for SSIs. Little research is available on the efficacy of various head covers in reducing the incidence of SSIs. Despite the lack of clear evidence, there is an ongoing disagreement over which form of head cover should be recommended in the perioperative setting. The American College of Surgeons guidelines indicate that skull caps with minimal hair exposure are acceptable, and the Association of Perioperative Registered Nurses recommends bouffant caps with coverage of all hair. In addition, they recommend covering the ears, sideburns, scalp, and nape of the neck, on the basis that hair and skin in these sites are known to harbor bacteria that can be dispersed.4, 5, 6, 7 However, no scientific evidence has shown a significant advantage in SSI reduction with either cap. This study aimed to determine the influence of surgical cap choice on SSI rates by comparing the incidence of SSIs based on attending surgeons’ use of skull caps or bouffant caps in the perioperative setting.
So how did the investigators, led by corresponding author Shanu N. Kothari, MD at the Gundersen Health System in La Cross, WI, approach this problem? Basically by reanalyzing data from a large randomized controlled trial that looked at whether clipping hair at the surgical site affected SSI rates. (It didn’t, by the way. The only reason we tend to clip hair these days is for convenience when there’s a lot of it.) Basically, data from this randomized study were re-analyzed to determine the impact of surgeon preference for bouffant vs skull cap, regardless of whether hair was clipped or left intact. In brief, patients were grouped based on the attending surgeons’ headwear, and the primary end point was SSI observed. Additional variables included preoperative comorbidities, operative approach, and procedure type.
Overall, there were 1,543 patients in the analysis, with attending surgeons wearing bouffant caps in 39% of the cases and skull caps in 61% of the cases. The authors found that patients whose surgeons wore a bouffant cap tended to be slightly older, have a lower BMI, and were undergoing primarily hernia/other procedures. Six patients in both the bouffant and skull cap groups had a history of colonization with methicillin-resistant Staphylococcus aureus (MRSA). Use of perioperative antibiotics were the same in both groups. The raw numbers showed that SSIs were observed in 96 (6.2%) of patients, with 8.1% in the bouffant group and 5.0% in the skull cap group. However, after adjusting for the type of operation and surgical approach in a multivariate logistic regression model, no difference in SSI rates for skull cap versus bouffant cap was detected.
This study has a lot of strengths. It was pretty large, with over 1,500 patients, and, because the study being reanalyzed was a study explicitly designed to examine SSI rates between a control and experimental group, the diagnostic criteria for SSI diagnosis were standardized and rigorous. Of course, its key limitation is that it is a post hoc analysis of an existing RCT dataset looking at a factor not incorporated into the previous design. The authors also noted:
The previous study data were biased toward male patients, as inclusion criteria consisted of adequate body hair to warrant hair clipping. Surgeon cap preference was linked with their specialty and procedure types. For example, the vast majority of foregut cases were performed by surgeons who preferred skull caps. In addition, although the head covering of the attending surgeon was known, we did not document the head coverings that other members of the surgical team wore. Also, the study was conducted in the setting of elective general surgical procedures and excluded vascular, anorectal, orthopaedic, obstetric, and gynecologic procedures. Analysis of cap material, including measures of pore size and comparison or particle counts, in addition to quantifying microbial sedimentation rate, were beyond the scope of this study.
Despite those limitations, when taken in the context of the evidence base existing before this study was carried out, these data are yet one more strong piece of evidence that choice of surgical headgear almost certainly doesn’t matter and doesn’t impact SSI rates. As the authors note, this is consistent with what we knew before, and this study isn’t alone. For instance, a large retrospective study by Shallwani et al failed to find a statistically significant change in the SSI rate from 13 months before to 13 months after the new AORN policies.
Tradition versus evidence in the operating room
One aspect of the study above that led me to learn more about this issue is a recent publication by Bartek et al, “Naked Surgeons? The Debate About What to Wear in the Operating Room“, which was cited by the authors. This particular opinion piece with targeted literature review pointed out how steeped in tradition, rather than evidence, so many infection control procedures in the operating room are and how heterogeneous and conflicting the evidence is for many of them. It’s a fascinating read and appears not to be behind a paywall; I recommend it.
Here’s an example that my UK colleagues might appreciate. It’s another AORN guideline that vastly differs from the recommendations in the UK, specifically the recommendation by AORN that all OR personnel keep their arms covered, amusingly under the topic of “The Right To Bare Arms”:
On the topic of covering the arms, AORN recommends: “When in the restricted areas, all nonscrubbed personnel should completely cover their arms with a long-sleeved scrub top or jacket” [1]. Interestingly, AORN’s recommendations and the United Kingdom’s NICE’s requirements are contradictory: As above, AORN recommends wearing a “long-sleeved scrub top or jacket,” whereas NICE’s policy is “bare below the elbows” [1, 22]. The fact that 2 large, guideline-producing bodies would recommend completely opposing practices under the rubric of evidence-based medicine is suspicious. Old studies looking at airborne bacteria show, among other things, that women wearing stockings shed more bacteria than women with bare legs [23]. NICE took the stance that handwashing is what is key and clothing with sleeves does not affect bacterial colony counts, but that it could affect practitioners’ abilities to wash their hands. This conclusion too has been refuted [7].
Perhaps some of my British colleagues who read this blog could chime in in the comments, but I must confess that I was amused by this controversy.
Bartek et al also note that, the further we dive into the question of bacterial shedding from people’s skin, the murkier things get. For example, they note that men shed twice as many bacteria as women, but no one has ever advocated for a restriction on men in the operating room. They also note that the release of bacteria from scrubs and street clothes was studied and found to be roughly equal; yet scrubs remain standard and street clothes are banned in the OR. Based on the previous findings, if decreasing SSIs is your goal there’s no real reason not to allow surgeons to come into the OR in their street clothes and to gown up over them, the very way surgeons were portrayed as doing in one of my favorite medical dramas of all time, The Knick. I also note that the surgeons in the year 1900 portrayed on The Knick also operated without gloves. (The wearing of sterile surgical gloves by surgeons and anyone who can touch the operative field is one of the few things that have been definitively shown to reduce SSI rates, a finding first reported by a protégé of William Stewart Halsted in 1899, a year before the fictional events portrayed in the first season of The Knick.)
Perhaps the most amusing observation was this:
Another set of studies reached an even more drastic conclusion: Naked men shed approximately a third to a half as many bacteria as the same men wearing street clothes or scrub suits [27, 28]. Perhaps “scrubs” actually live up to their name: rather than “catching” squames, which the skin sheds perpetually, they may in fact be “scrubbing” these bacteria-laden squames from our skin. If we are to adhere to the strict prescription of evidence-based medicine, ought we to disrobe prior to entry into the operating room? We argue no, although for reasons that are outside of how it would affect bacterial counts in the operating room.
Who says there’s no room for humor in the peer-reviewed medical literature?
There are other common practices that really don’t have a strong evidence base for them. (Some would even argue that the surgical site classification is lacking in that respect.) For instance, there is no evidence that wearing surgical masks prevents SSIs. Indeed, there’s even a Cochrane review that suggests otherwise, and Bartek et al point out that masks have never been shown to be effective in preventing SSIs. However, if your purpose is to protect the surgeon and others working on the patient from being splattered with blood in the mouth or nose, then requiring surgical masks makes perfect sense, just as requiring protective eyewear does. That’s likely why no one is proposing that we surgeons stop wearing them. Certainly, as someone who’s been sprayed in the face with blood many times over the years (although much less frequently and with much less volume ever since I restricted my practice to breast surgery), I’m grossed out by the thought of operating without a mask.
The bottom line is that, although the reaction of surgeons and the ACS to the AORN recommendation struck me as rooted far more in emotion and tradition than anything else, the ACS did have a point. There was no evidence that choice of headgear has a significant impact on SSI rates, and there is no evidence that it does. In its response to the AORN guidelines ACS would have been better served by ditching the bit about the skull cap being a “symbol” of the surgical profession, which struck me as a callback to our more-than-a-bit sexist past, and sticking to the evidence. Similarly AORN would have done well not to overreach and extrapolate beyond what the evidence justified in its recommendations. Finally, I can’t help but conclude that this entire kerfuffle was an example of how the smallest disagreements all too often result in the most protracted fights.