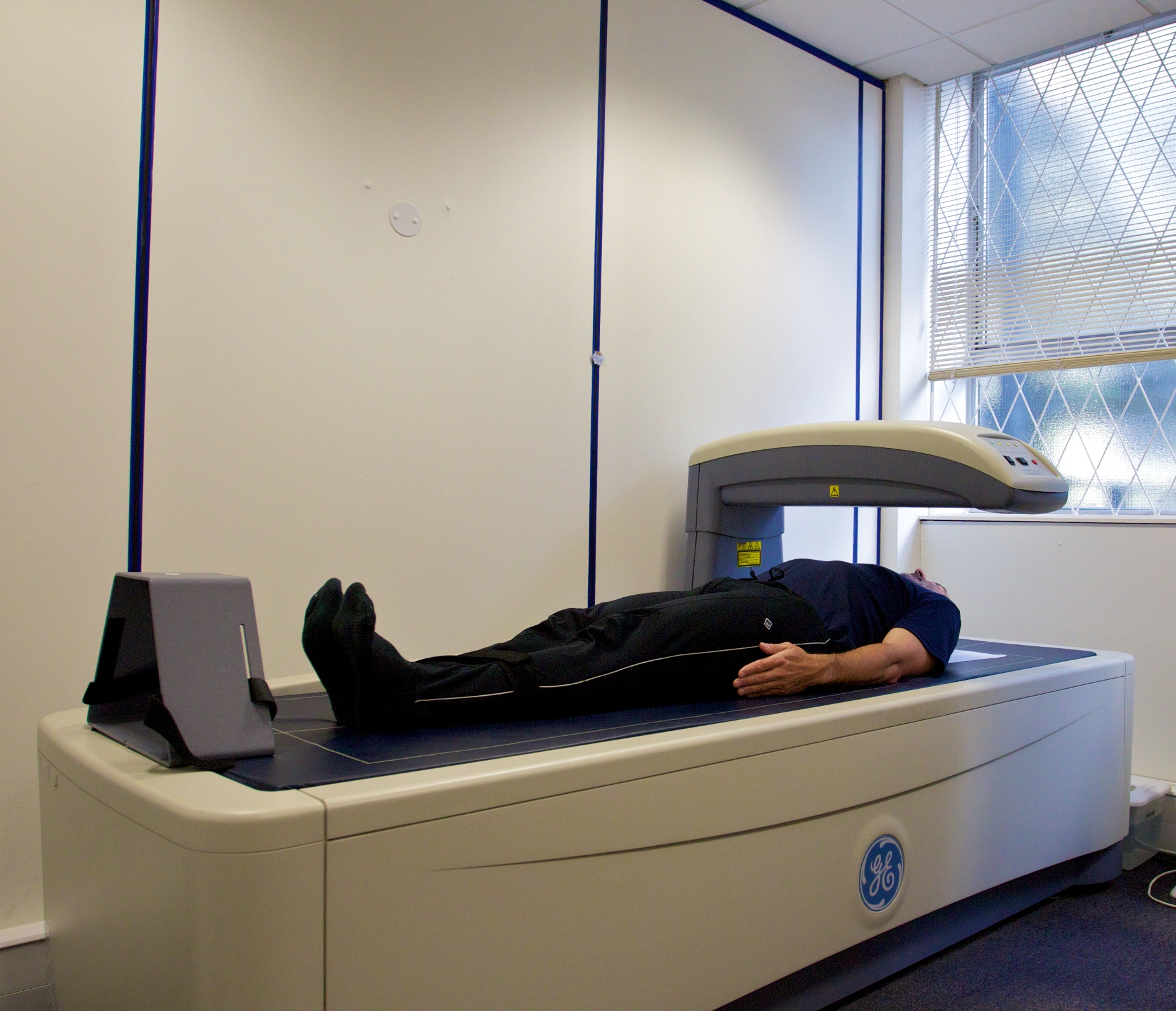
DEXA Scanner Measures Bone Mineral Density
Bisphosphonate drugs have been shown to increase bone density and prevent fractures in postmenopausal women with osteoporosis (remember Sally Field in those ads for Boniva?) but what about women with milder decreases in bone density (osteopenia)? Can the drugs prevent osteoporosis and/or fractures in patients with osteopenia?
A recent study published in The New England Journal of Medicine set out to answer that question. “Fracture Prevention with Zoledronate in Older Women with Osteopenia.” was a 6-year randomized, placebo-controlled, double-blind trial of 2,000 women age 65 or older with osteopenia (defined as a T-score of -1.0 to -2.5). Subjects received four IV infusions of either zoledronate or saline at 18-month intervals. Those who got zoledronate had significantly fewer vertebral and non-vertebral fragility fractures. But there was no significant decrease in hip fractures. They estimated that the number needed to treat (NNT) to prevent one (non-hip) fracture in one woman was 15.
While it is disappointing that the treatment had no effect on hip fractures, these are nevertheless impressive results, and the NNT is better than for many of our other standard treatments. Does this mean we should identify all older women who have osteopenia and treat them with IV zoledronate every 18 months to prevent fractures? I think it is too soon to jump on that bandwagon. There are a lot of unanswered questions.
Is osteopenia a disease that needs treating?
Osteopenia is defined as lower than average bone density; it is a risk factor for developing osteoporosis. It can be considered a normal consequence of aging, affecting over half of women older than 50. What defines a disease? Many lab values like estrogen and testosterone levels decrease with age; when do they become a disease that needs treating? The majority of women with osteopenia will not go on to develop osteoporosis, and not all those with osteoporosis will have fractures. Hip fractures are devastating, leaving many women bedridden and shortening their lives; but two thirds of vertebral fractures are asymptomatic. Is it reasonable to lump them together?
Fragility fractures are fractures that occur from a fall from a standing height or less. An article in The BMJ pointed out that fragility fractures are not always osteoporotic fractures; we may be overdiagnosing bone fragility in the quest to prevent hip fractures.
In 2008, The BMJ published the article “Drugs for pre-osteoporosis: prevention or disease mongering?” Not long after, the drug manufacturer Merck was accused of inventing the disease osteopenia in order to sell its drug Fosamax. I wrote about that controversy in 2010.
How is it diagnosed?
Dual Energy X-ray Absorptiometry (DEXA) is the test most commonly used to measure bone mineral density (BMD) and to diagnose osteoporosis. It involves a low dose of radiation.
BMDs are given a T-score, a standard deviation-based comparison to the BMD of a healthy 30-year-old of the same race and sex.
| Bone Density (BMD) | T-Score | Prevalence (%)* |
| Normal | +1.0 to -1.0 | 20 |
| Low (osteopenia) | -1.0 to -2.5 | 52 |
| Osteoporosis | -2.5 or more | 28 |
*in white women older than 50
These categories were arbitrarily assigned by the World Health Organization (WHO) and were meant to be a tool to measure the emergence of a problem in a population. They were not meant to diagnose individuals, but they are being used that way. The definition of osteopenia starts when the bone density is one standard deviation below the average for a young woman. Some women diagnosed with osteopenia may just be on the low end of the normal spectrum. These scores have been interpreted to mean that half the population has a disease they need to worry about.
The emphasis has been on women. If men’s bones are compared to the BMD of a 30-year-old white man, nearly half of all middle-aged men would be diagnosed with osteopenia, but their risk of hip fractures is much lower than for women. And in a Merck study, the prevalence of osteopenia varied from 28% to 45% depending on the machine being used.
Bone density doesn’t capture a poorly understood factor known as bone quality, which declines with age. Given the same bone density, an 80-year-old woman is at much greater risk of a fracture than a 50-year-old.
Other risk factors for fracture
Other risk factors include:
- Gender (women are at higher risk, especially after menopause)
- Race (Asian and Caucasian women have higher risk)
- Family history can increase risk by 50-85%
- Age (BMD decreases by 0.5% every year after age 50)
- Lifestyle choices (poor diet, excessive alcohol or caffeine, lack of exercise)
- Bone structure and body weight (petite and thin women at greater risk)
- Smoking
- Other medical conditions
- Certain medications
The FRAX tool takes many but not all of these risk factors into consideration then estimates the 10-year probability of hip fracture or major osteoporotic fracture.
Recommendations for screening and treatment
The USPSTF recommends screening for bone density in women age 65 and up and in postmenopausal women younger than 65 who are at increased risk of osteoporosis. It does not recommend screening men.
The National Osteoporosis Foundation recommends treatment for postmenopausal women and for men over 50 who have:
- Prior hip or vertebral fracture
- T-score of −2.5 at the femoral neck or spine, excluding secondary causes
- T-score between −1.0 and −2.5 at the femoral neck or spine and a 10-year probability of hip fracture ≥3% or a 10-year probability of major osteoporotic fracture ≥20%
- Clinicians’ judgment in combination with patient preferences indicate treatment for people with 10-year fracture probabilities above or below these levels.
The first two are diagnostic of osteoporosis. Number 3 is based on osteopenia. The last item is important. The clinician can consider other relevant details like the degree of trauma associated with a prior fracture, the patient’s exercise history, family history, the patient’s willingness to accept the risks, financial considerations (each infusion costs $1,200), whether the patient engages in activities where falls are likely, etc.
Questions about the new study
In the first place, it is never wise to let a single study guide clinical practice, since there are so many things that can go wrong in research. It would be reassuring to have other studies with similar findings.
According to The Medical Letter, the FDA has approved IV zoledronic acid every two years to prevent osteoporosis in women with osteopenia. Approval was based only on improvements in BMD; until this new study, there was no available evidence for a reduction in fractures.
The new study found a reduction in fractures, but there was no reduction in hip fractures, the fracture of most concern. Why wouldn’t an improvement in bone density have the same effect on all fractures anywhere in the body?
The study participants had a T-score of -1.0 to -2.5 at either the total hip or the femoral neck on either side. Some subjects were “at the interface between osteopenia and osteoporosis.” If they had a T-score of less than -2.5 in the spine or at the hip/femoral neck on one side they were not excluded. This muddies the findings. I wish they had excluded everyone with even a single finding of a T-score below -2.5. And it raises the question of which BMD measurement is the most reliable for screening.
Which bisphosphonate?
Bisphosphonates are recommended as first-line treatment for osteoporosis. There are several to choose from. Some have been shown to reduce the risk of vertebral and hip and other nonvertebral fractures in osteoporosis; ibandronate has only been shown to reduce the risk of vertebral fractures. Drugs other than zoledronic acid (Zoledronate, brand name Reclast) have not been shown effective for osteopenia. There have been no head-to-head trials comparing different bisphosphonates. Oral bisphosphonates require special precautions; patients must fast overnight, take the drug with 6-8 ounces of plain water, avoid ingesting anything other than plain water for 30 minutes, and remain in an upright position for 30-60 minutes. IV versions are more acceptable to patients.
What are the risks?
A number of side effects have been reported with bisphosphonates, including vision problems, cough, headache, muscle pain, GI disturbances, jaw osteonecrosis, long-bone fractures and atrial fibrillation. IV infusions have caused reactions (flu-like symptoms and more), usually with the first infusion; these reactions can sometimes last for months. There have been no long-term follow-up studies.
What have other studies of bisphosphonates found?
In a randomized, double-blind, placebo-controlled trial of patients who had surgical repair of a hip fracture, a yearly injection of zoledronic acid reduced the incidence of new clinical vertebral fractures from 3.8% to 1.7%, of new nonvertebral fractures from 10.7% to 7.6%, and of deaths from any cause from 13.3% to 9.6%. The incidence of hip fractures was reduced, but the reduction was not statistically significant. Only 41-42% of subjects had a T-score of -2.5 or less.
The majority of fractures occur in women with osteopenic T-scores because there are far more women in that group. The fracture rate rises progressively with decreasing BMD scores. The number needed to treat (NNT) to prevent one fracture was reportedly much higher for osteopenia (>100) than for osteoporosis (10-20). This article went on to say it is not advisable to treat patients based on T-scores alone.
The NNT website got very different results for bisphosphonate treatment of women without prior fractures. NNT: no fractures were prevented. NNH: a small number were harmed. They got their data from the Cochrane Database of Systematic Reviews. They say, “…in those without very low BMD or fractures no study has demonstrated a true benefit.” And they point out flaws in the positive studies reviewed by Cochrane: for one drug there was only a single study, subgroup analyses were used, and the fractures were diagnosed by x-ray and may not have been clinically significant.
Conclusion: Useful, but not for everyone
Bisphosphonates are undeniably useful for patients with osteoporosis, but it has not yet been established which patients with osteopenia will benefit. The NNT website warns:
serious side effects such as atypical fractures and osteonecrosis of the jaw and gastrointestinal, musculoskeletal, and other side effects leading to disproportionate discontinuation have been increasingly linked to use of these drugs in the long term. These side effects should strike a note of caution and should firstly be discussed with any woman considering bisphosphonate therapy, and secondly be a warning against initiating this therapy in patient groups who have not been proven to benefit.
As I said in my 2010 article,
Sally Fields sends a panacea message rather than saying this is a drug with pros and cons that only offers partial protection and doesn’t benefit every woman who takes it, and that shouldn’t automatically be prescribed to everyone diagnosed with osteopenia by an arbitrary test.
Bottom line: patients are complicated individuals, and knee-jerk one-size-fits-all cookbook prescriptions are not justified. We should look at clinically significant benefits, not just test results. For statins, we don’t just want improved cholesterol levels, we want to see fewer heart attacks, strokes, and deaths. For bone density, we don’t just want improvements in T-scores; we want to see fewer osteoporotic fractures, particularly fewer hip fractures. Questions remain; more research will be useful in guiding clinicians.

